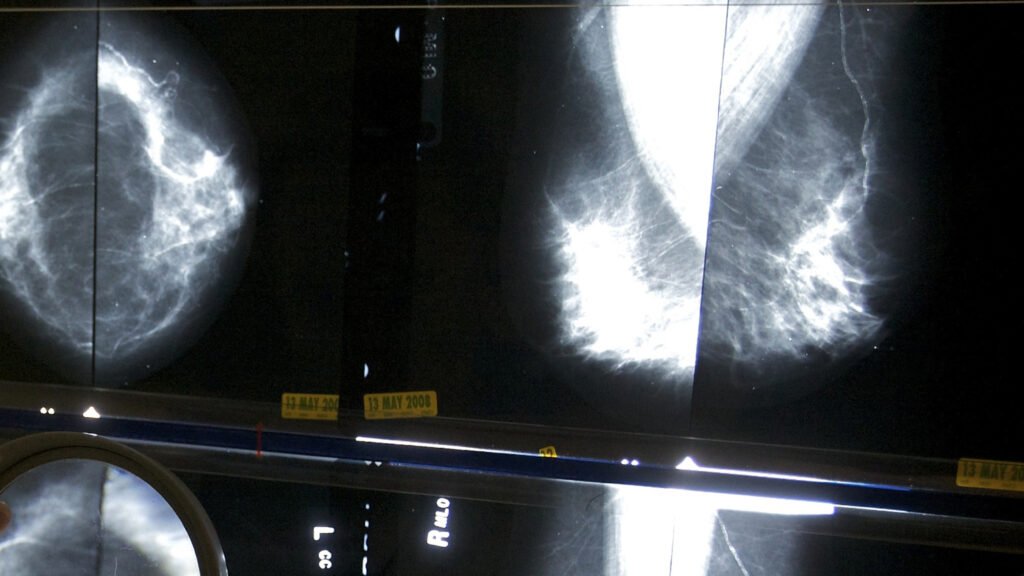
WASHINGTON — Deciding when to get a routine mammogram can be confusing. Some health organizations recommend that women start at age 40 or 45, while others have recently chosen age 50. Opinions also differ as to whether annual or biennial is best.
This contradictory advice is, at least in part, because breast cancer screening guidelines are designed for women who are at average risk and have no possible symptoms of cancer. But because breast cancer is so common, it’s difficult to know who is truly “average” and how to balance the pros and cons of screening.
“Breast cancer is not one disease,” says Dr. Laura Esserman of the University of California, San Francisco. “So what’s the point in testing everyone the same way if everyone doesn’t have the same risk?”
Esserman is leading research to better understand the nuances of who is at low risk, high risk, and somewhere in between, and ultimately provide more tailored screening advice.
According to the American Cancer Society, more than 320,000 women in the United States will be diagnosed with breast cancer this year. Mortality rates have been declining for decades, primarily due to improved treatments. However, cancer remains the second leading cause of cancer death among women in the United States, and the number of diagnoses is slowly increasing.


STAT Plus: The AI industry wants to turn routine mammography into a powerful multi-tool
For now, there are a few things you need to know.
When to get a mammogram
The most recent guidance comes from the American College of Physicians, which recommends that average-risk women ages 50 to 74 get a mammogram every other year. The guidelines say people between the ages of 40 and 49 should discuss the pros and cons with their doctors and get tested every other year if they choose to be tested.
That advice, issued last month, was surprising. Most other U.S. health organizations urge women to start earlier, in their 40s. The influential U.S. Preventive Services Task Force recently changed its guidelines to start biennial mammograms at age 40 instead of age 50.
The American Cancer Society has long recommended that women between the ages of 45 and 54 get an annual mammogram, but says women can choose to start at age 40. Women over 55 can choose to switch to every other year or continue getting tested every year, the cancer society said.
The American College of Physicians’ new guidelines also say doctors can ask women over 75 if they would like to cancel routine exams. In contrast, the Cancer Society argues there is no reason to stop if the cancer is still healthy.
Why don’t the experts agree?
The higher a woman’s risk of eventually developing breast cancer, the greater the benefit from having more frequent screenings. But aside from a few well-known factors, such as the cancer-causing BRCA1 and BRCA2 genes, it’s difficult for women to know their true risk. Age has long been considered a surrogate factor, as women’s risk of breast cancer increases as they age.
Mammography isn’t perfect. Cancer may be missed or a malignant tumor may appear after a routine mammogram. But the guidelines try to balance the benefits of detecting cancer early with the potential harms, such as stress and pain, of investigating suspicious areas that are not known to be cancerous.
Dr. Carolyn Crandall of the University of California, Los Angeles, who chaired the American College of Physicians’ report, cautioned that mammography in the 1940s was “not to say it didn’t have benefits.” However, “the balance between benefits and harms for people aged 40 to 49 is narrower.”
The American Cancer Society recommends starting mammography every year starting at age 45. That’s because the incidence of breast cancer among people aged 45 to 49 was found to be higher than among those in their early 40s, which is similar to the incidence of breast cancer among those aged 50 to 54, said public health researcher Robert Smith, the society’s early cancer detection expert.


STAT Plus: AI could check millions of CT scans for heart risks. Who will pay for it?
What’s missing, Smith noted, is a way to know whether a person is more likely to develop an aggressive form of breast cancer or a slower-growing form of breast cancer.
Impact of dense breasts on mammography advice
Almost half of women over the age of 40 have dense breast tissue, which can make it harder to find tumors on mammograms and slightly increase the risk of developing cancer.
After a mammography test, a woman will be informed about her breast density. Many experts say it’s not yet clear whether women with dense breasts would benefit from adding ultrasound or MRI to their screening. But new guidance from the American College of Physicians recommends considering 3D mammography (what doctors call digital breast tomosynthesis, or DBT).
Future issues in breast cancer screening
In the future, adding genetic tests that look beyond the well-known BRCA genes, along with a broader range of risk factors, may help improve a woman’s optimal mammography schedule.
A recent study of about 46,000 women, called the WISDOM trial, used age, genetic testing, lifestyle, health history, and breast density to categorize women as low-risk, average-risk, high-risk, or high-risk. This risk level determined whether women should wait until age 50, have a mammogram every other year, or every year, with the highest-risk group told to have two mammograms and two MRI scans a year. We compared risk-based scans to standard annual mammography.
Risk-based screening was as effective as annual screening, Esserman’s team reported in the medical journal JAMA. One surprise: About 30% of women whose genetic testing showed an increased risk did not report having any relatives with breast cancer. More research is underway, but Esserman expects early findings to start influencing guidelines soon.
It’s also developing AI tools to assess a woman’s risk of developing breast cancer in the next few years based on mammography clues, another way to identify people who might be candidates for more or less frequent screening.
For now, women can talk to their doctors about other risk factors, such as close relatives who have had cancer, their own overall health, whether they’ve had children, and at what age they had them.
The cancer society’s Ms Smith said that no matter what age or interval you choose for breast cancer screening, the best advice is to stick to it: “Breast cancer screening is most effective when done regularly.”
— Laurent Neergaard
The Associated Press Health and Science Department receives support from the Howard Hughes Medical Institute’s Department of Science Education and the Robert Wood Johnson Foundation. AP is solely responsible for all content.