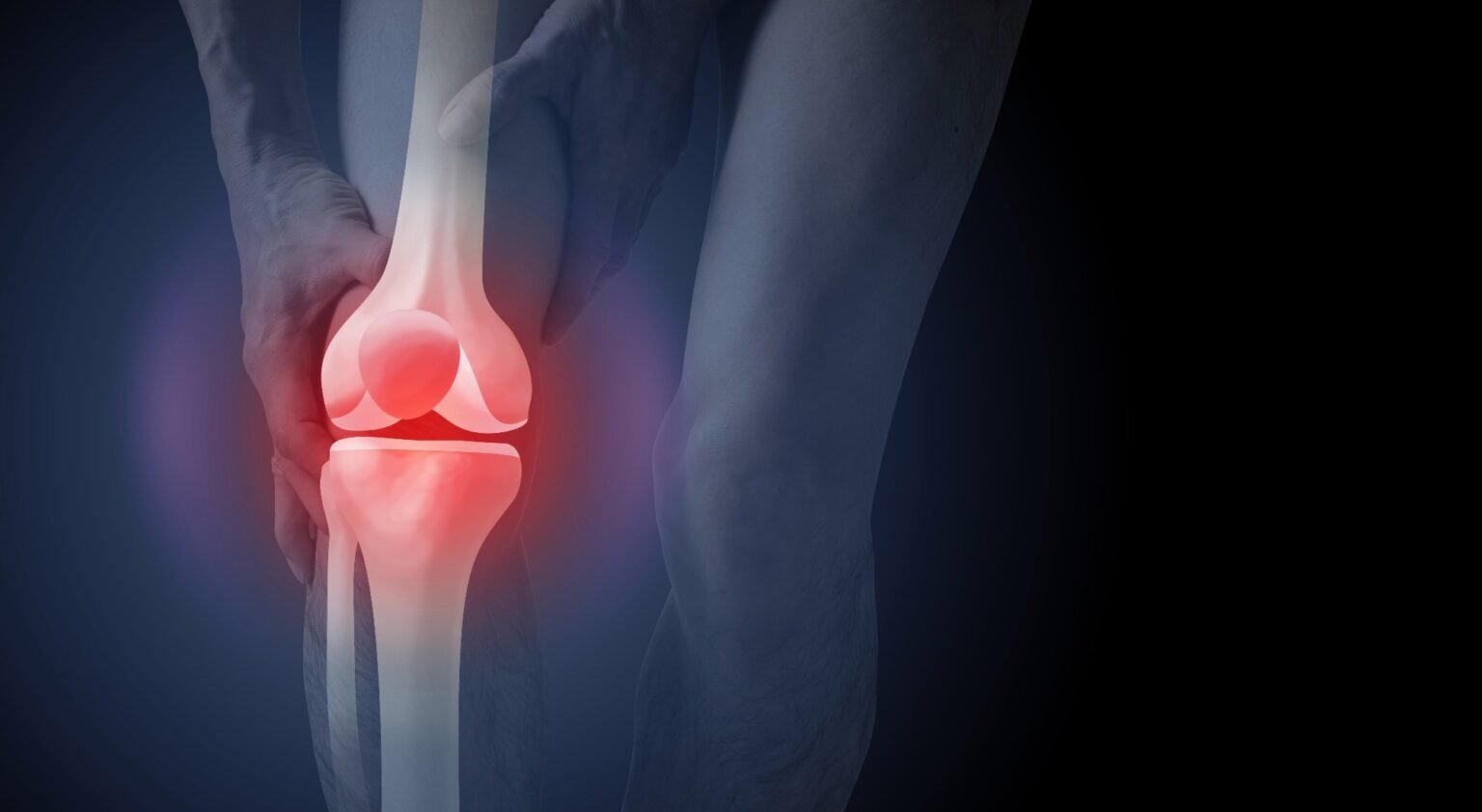
A new MRI study suggests that a diet high in ultra-processed foods may be associated with thicker, poorer thigh muscles in adults at risk of knee osteoarthritis, adding new concerns about how modern dietary patterns affect mobility and aging.
Study: Ultra-processed foods and muscle fat infiltration in thigh MRI: data from the Osteoarthritis Initiative. Image credit: Atiketta Sangasaeng / Shutterstock
Recent research published in journals Radiology Consumption of ultra-processed foods (UPF) is associated with increased fat infiltration in the thigh muscles on magnetic resonance imaging (MRI), a marker of decreased muscle quality in people at risk for knee osteoarthritis.
Analysis of MRI data from 615 participants showed that higher UPF intake was associated with greater fatty infiltration of the thigh muscles, even after accounting for body mass index (BMI), and a stronger association when accounting for abdominal circumference (AC).
These findings suggest that diet quality and fat distribution may be associated with lower thigh muscle composition, regardless of gender, especially in older adults who are at risk for functional decline.
UPF, a feature of the modern Western diet, contributes significantly to the rise in obesity rates. These products, which are high in salt, sugar, fat, and additives, are often substituted for nutritious foods, resulting in poor diet quality and insufficient intake of protein and important micronutrients essential for muscle health.
Obesity is a major risk factor for knee osteoarthritis (KOA), a disabling condition that affects multiple joint tissues, including muscle and fat.
Emerging evidence shows that increased UPF intake is associated with worse knee outcomes, decreased physical performance, decreased muscle mass, and increased body fat. However, its impact on skeletal muscle integrity is still poorly understood, especially in individuals at risk for KOA.
MRI study design for UPF and knee osteoarthritis
In this study, researchers examined the association between UPF intake and thigh muscle fat infiltration (MFI) in Osteoarthritis Initiative (OAI) study participants from 2004 to 2015.
Although these people were more likely to have KOA, they did not have radiographic osteoarthritis (grade 1 or less on the Kellgren-Lawrence scale) and did not report joint pain, stiffness, or major comorbidities (inflammatory arthritis, diabetes, stroke, or cancer).
The team assessed dietary intake using validated food frequency questionnaires (FFQs), including the Block Brief 2000 FFQ, and recorded food consumption over the previous year. They used the NOVA system to classify foods and estimate UPF intake.
To assess muscle quality, the researchers analyzed axial MRI slices. They used the Goutallier classification to rank MFIs. Grades ranged from 0 (cases with no fatty infiltration) to 4 (cases with >50% fatty infiltration). Two experienced readers independently scored 10 bilateral thigh muscles to generate a total score for flexor, extensor, adductor, and total thigh MFI.
The researchers used two regression models, one adjusted for BMI and one adjusted for AC. Both models were further adjusted for age, race, ethnicity, education, income, physical activity, total energy intake, depression, and smoking status.
Additionally, the team conducted gender-stratified and sensitivity analyzes by adjusting for total dietary fat and comparing participants without radiographic KOA (grade 0) with those with suspected KOA (grade 1). To ensure reliability, both readers rescored a subset of 100 participants after 6 weeks to assess reproducibility.
Higher UPF intake and muscle quality findings
The study population consisted primarily of older women (mean age 60 years), women (n=340), and non-Hispanic ethnicity (98%). Most of them were overweight with an average BMI of 27, and more than half reported never smoking. Abdominal obesity was common, affecting 43% of men and 81% of women (mean AC, 99 cm). The average energy intake was 1,381 kcal/day, and UPF accounted for approximately 41% of the daily intake.
After adjusting for BMI, higher UPF intake was significantly associated with increased femoral MFI in all thigh muscles and bilateral flexor and adductor muscles. These associations were stronger in models adjusted for waist circumference than in models adjusted for BMI.
The results of this study suggest that while central fat distribution may help explain this relationship, UPF intake may also be associated with muscle fat accumulation.
Together, these support an association between poor diet quality and increased intramuscular fat in this at-risk population, although the underlying mechanisms were not directly tested in this study.
The relationship between UPF consumption and MFI was linear and consistent across genders. Among muscle groups, flexors showed the highest MFI, extensors the lowest MFI, and adductors showed the strongest association with UPF intake. Reproducibility analysis showed good interobserver and intraobserver agreement for Gutallier grading.
Sensitivity analyzes confirmed the robustness of the findings, with adjustments for total dietary fat remaining unchanged and showing a stronger association among people with suspected KOA than among those without radiographic disease. However, as a cross-sectional study, this result does not establish a causal relationship.
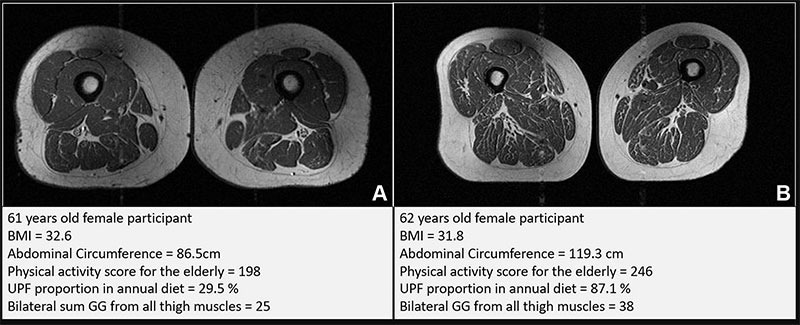
Representative axial T1-weighted spin-echo femoral MRI scan (A) With a 61 year old female participant (B) A 62-year-old female participant. Both participants were of similar age and body mass index (BMI, calculated as weight in kilograms divided by height in meters). Both had scores on the Physical Activity Scale for Older Adults that were above the average score in the study. According to the World Health Organization definition, participants B Recognized as having abdominal obesity (waist circumference ≥88cm). Waist circumference is a measure of central obesity that captures fat distribution and serves as an indicator of cardiometabolic health. Compared to the participants aparticipants of B The proportion of ultra-processed foods (UPF) in the diet was higher (87.1% vs. 29.5%), the thigh muscles on both sides were thicker, and the sum of the Goutalier grade (GG) of all thigh muscles in participants was 25. a Participants: 38 B. Image: Radiological Society of North America (RSNA)
Diet quality and its impact on musculoskeletal health
This study identifies that the consumption of ultra-processed foods is associated with decreased muscle quality, which is reflected in increased fat infiltration in the thigh muscles of people at risk for knee osteoarthritis, regardless of gender.
The stronger association in the waist circumference-adjusted model highlights the potential for diet quality and fat distribution to jointly influence musculoskeletal health.
Although this finding supports further research into whether dietary patterns influence age-related muscle quality and functional decline, future longitudinal studies will be needed to clarify the causal pathways and determine whether dietary interventions can reduce muscle deterioration and slow the progression of KOA.