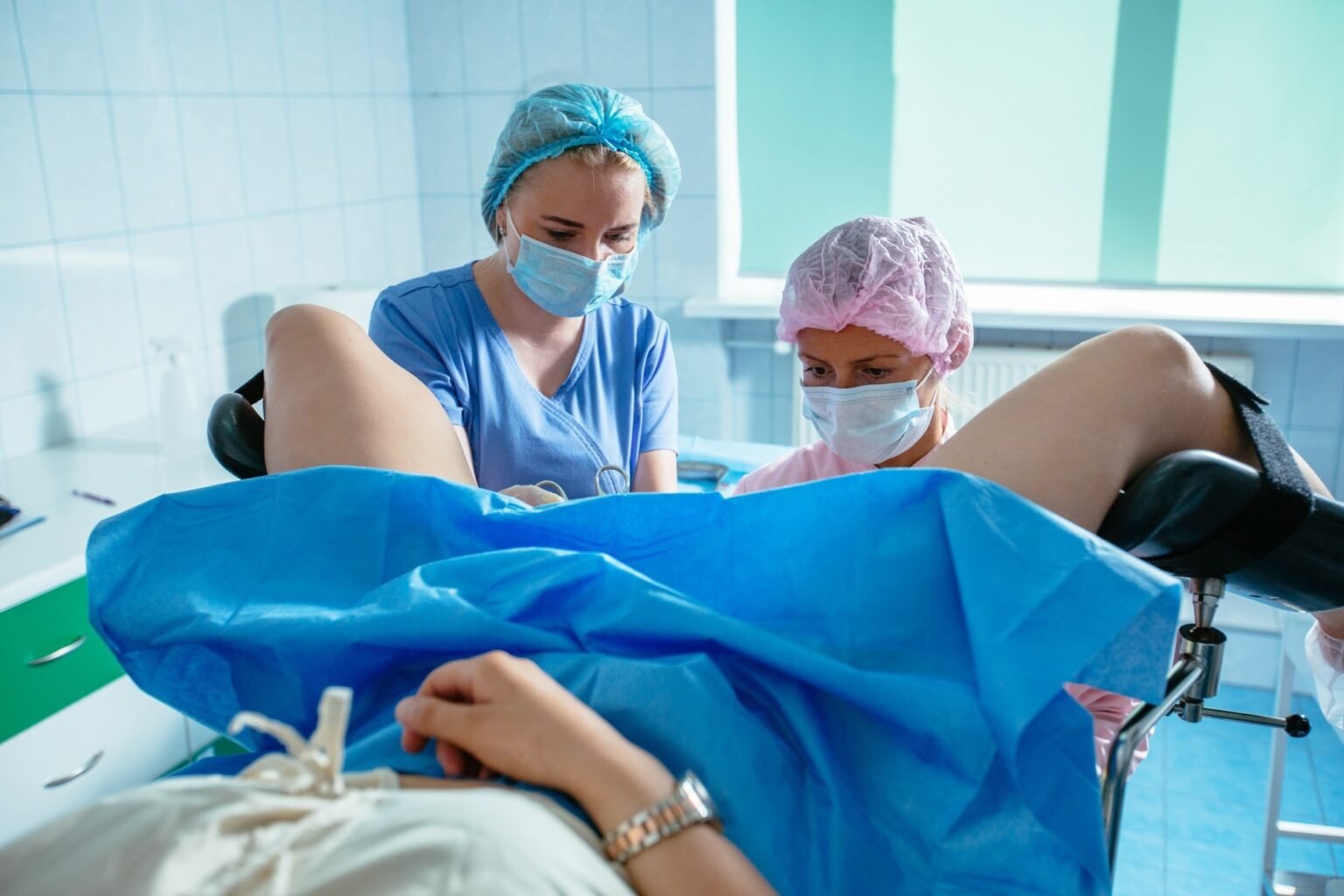
Thousands of real patient testimonies reveal how inconsistent care, ignored pain, and unequal treatment continue to shape women’s experiences with common but often painful procedures.
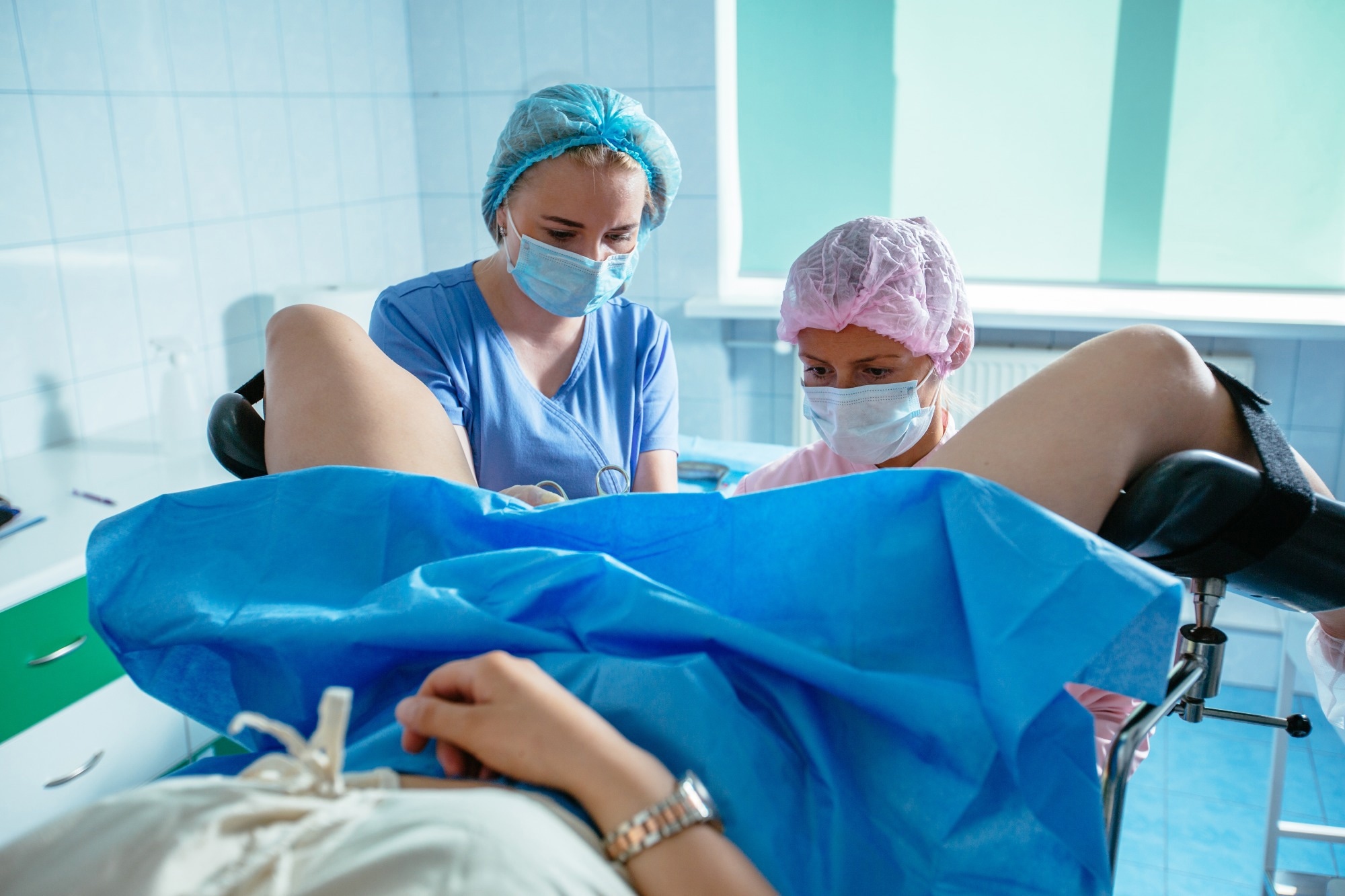 Research: From pain gaslighting to gender bias in women’s descriptions of hysteroscopies: A qualitative reflexive thematic analysis. Image credit: Iryna Inshyna/Shutterstock.com
Research: From pain gaslighting to gender bias in women’s descriptions of hysteroscopies: A qualitative reflexive thematic analysis. Image credit: Iryna Inshyna/Shutterstock.com
new women’s health This study analyzed impromptu real-life conversations shared on Mumsnet to explore the clinical, organizational, and personal factors that shape women’s hysteroscopy experiences.
The need to improve the provision of hysteroscopy services
Hysteroscopy is a common medical procedure in which a doctor examines the uterus. This is often the first step in evaluating symptoms such as irregular or heavy periods. In the UK, hysteroscopy is called outpatient hysteroscopy (OPH) and is primarily performed on an outpatient basis. Approximately 71,000 surgeries are carried out in the UK each year.
Hysteroscopy is considered the gold standard for visualizing the uterine cavity. However, there is significant heterogeneity in success rates (77% to 97.2%). Failure to complete OPH is primarily related to pain during the procedure. More than 85% of patients experience pain, with 15% to 34.8% of women reporting severe pain. Some reports provide insight into pain and satisfaction during and after the procedure, but may not provide an overall view of the true impact of the procedure.
There is a lack of research on the actual treatment experience of hysteroscopy, which limits the ability to translate patient experience into clinical improvements. The Royal College of Obstetricians and Gynecologists (RCOG) recommends qualitative research to incorporate patient perspectives into clinical care. A rich source of qualitative data are the online discussion forums that women often use to share their experiences and seek advice. These discussion forums may provide new insights that may help improve the quality of our Services.
Evaluate the Mumsnet dataset to identify key patterns and insights
Mumsnet is a UK-based parenting site. The number of monthly posts is 700,000, and the number of monthly visits is 33.1 million. Around 52.6% of users identify as female, and accounts shared on Mumsnet include opinions from across the UK. Posting and replies are unprompted and not researcher-driven.
Data were extracted for the period March 4, 2018 to December 31, 2024, and all posts related to issues other than hysteroscopy were excluded. Across 1971 users, 4769 posts were scraped, leaving 4644 posts from 261 threads after exclusion. Forums often contain multiple points of view on a topic. The analysis conducted was reflexive and thematic, capturing the depth and diversity of the conversations and focusing on the coherence of the analysis.
Five themes were constructed to represent women’s specific experiences in the hysteroscopy trajectory: conditional consent, unrecognized vulnerability, pain roulette, gynecological pain gaslighting, and gender pain gap.
Clinical blind spots influence the perception of neglect in OPH
Regarding conditional consent, patients received insufficient information and were unable to make an informed choice. As a result, I often felt hurt and disappointed. As OPH was presented as the only timely intervention strategy, consent was often given out of fear of symptom progression and necessity rather than genuine desire. Withdrawing consent was difficult due to overt pressure from clinicians, fear of worsening pain, and inaccurate information.
The intimate nature of the procedure made women feel physically and mentally vulnerable, and comments from users highlighted the power imbalance between clinician and patient. Comparisons were made with sexual violence, with patients with a history of sexual abuse reporting increased feelings of vulnerability. Side effects lasted for a long time, interfered with help-seeking behavior, and resulted in patients being more clinically vulnerable overall.
Discrepancies in the administration of general anesthetics (GA) and over-the-counter (OTC) analgesics have been reported. Significant heterogeneity in pain management was observed between trusts and hospitals. This discrepancy led patients to believe that their pain relief options depended on luck, reinforcing a sense of unfairness. Forum users also expressed concern about the lack of more options for pain management, although they acknowledged the difficulty of standardizing painkillers.
Forum users also alluded to stigmatization by medical professionals and the systematic minimization and dismissal of their concerns (‘gaslighting’). The validity of women’s pain experiences was questioned, and in some cases, medical records were reported to be inconsistent with patients’ actual experience at the time of the initial hysteroscopy. During the waiting phase, hysteroscopy was positioned as “acceptable for most people,” which felt inauthentic to forum users.
The data demonstrate a recognition of gender bias in medicine, where historical assumptions about women’s pain were considered outdated. A fundamental disparity in pain perception was observed between male and female patients. Forum users also suggested the use of distraction techniques to manage pain rather than effective pain relief. Other concerns centered on the infantilization of women, mistrust, and a deep sense of discrimination. Normalizing women’s pain creates unequal standards of pain management and leads to a lack of trust in the health care system.
conclusion
The current study used qualitative data to detect clinical blind spots in OPH around five themes: conditional consent, unrecognized vulnerability, pain roulette, gynecological pain gaslighting, and gender pain gap. These insights should help devise reforms to ensure more equitable, progressive, patient-centered, and responsible treatment strategies for women.
However, the authors note that negative experiences can be overrepresented in online accounts, and that experiences with hysteroscopies vary widely, with many women accepting the procedure in some circumstances. Therefore, the findings should be interpreted as a contextual account, rather than representative of all patient experiences or prevalence, and highlight broader systemic and organizational variables in care rather than uniformly poor care.
Click here to download your PDF copy.