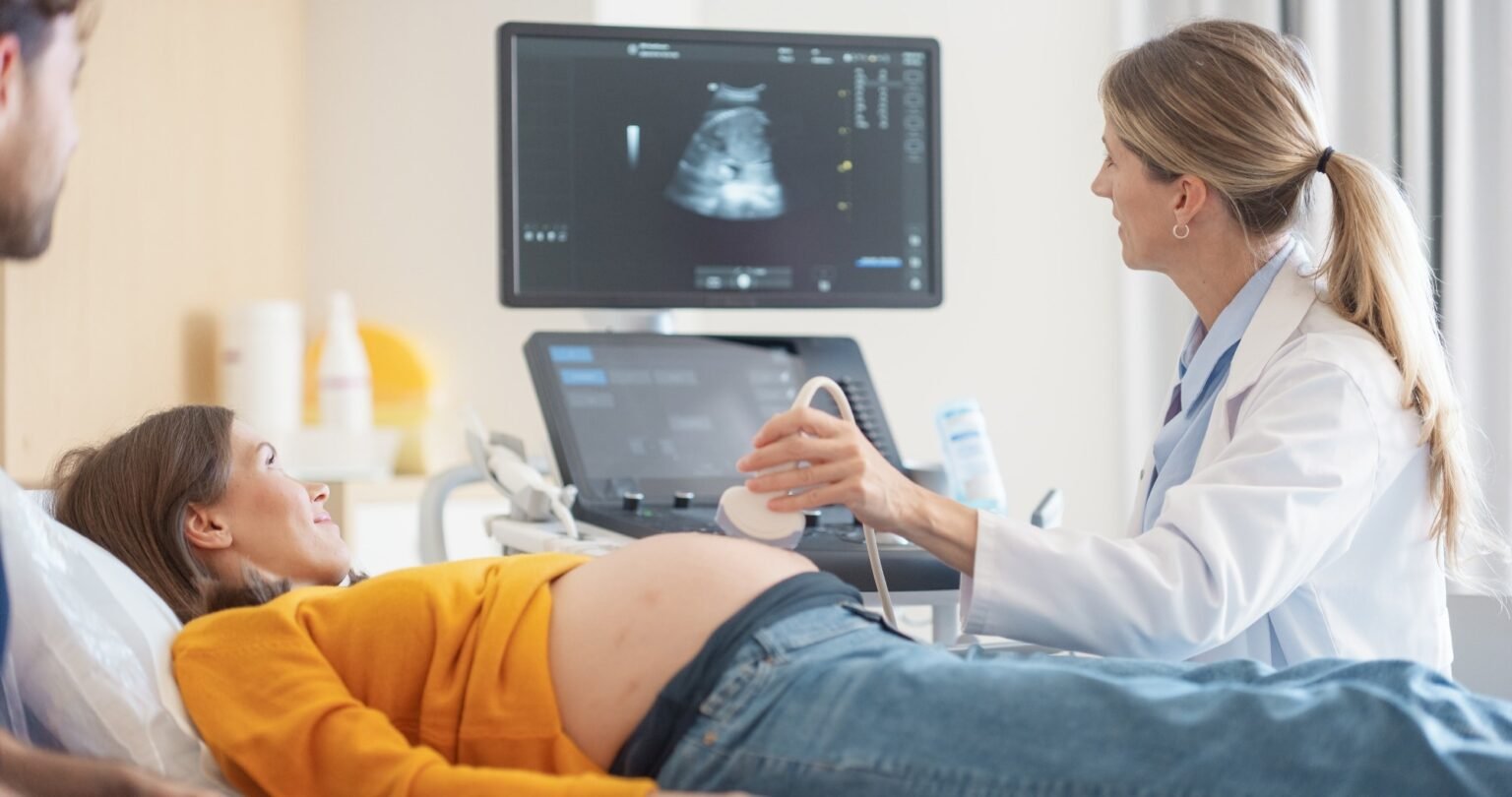
New Ontario data shows that pregnant doctors often take on more work during the first trimester and then take more variable and short parental leave, raising urgent questions about medical culture, workforce planning and gender equity in health care.
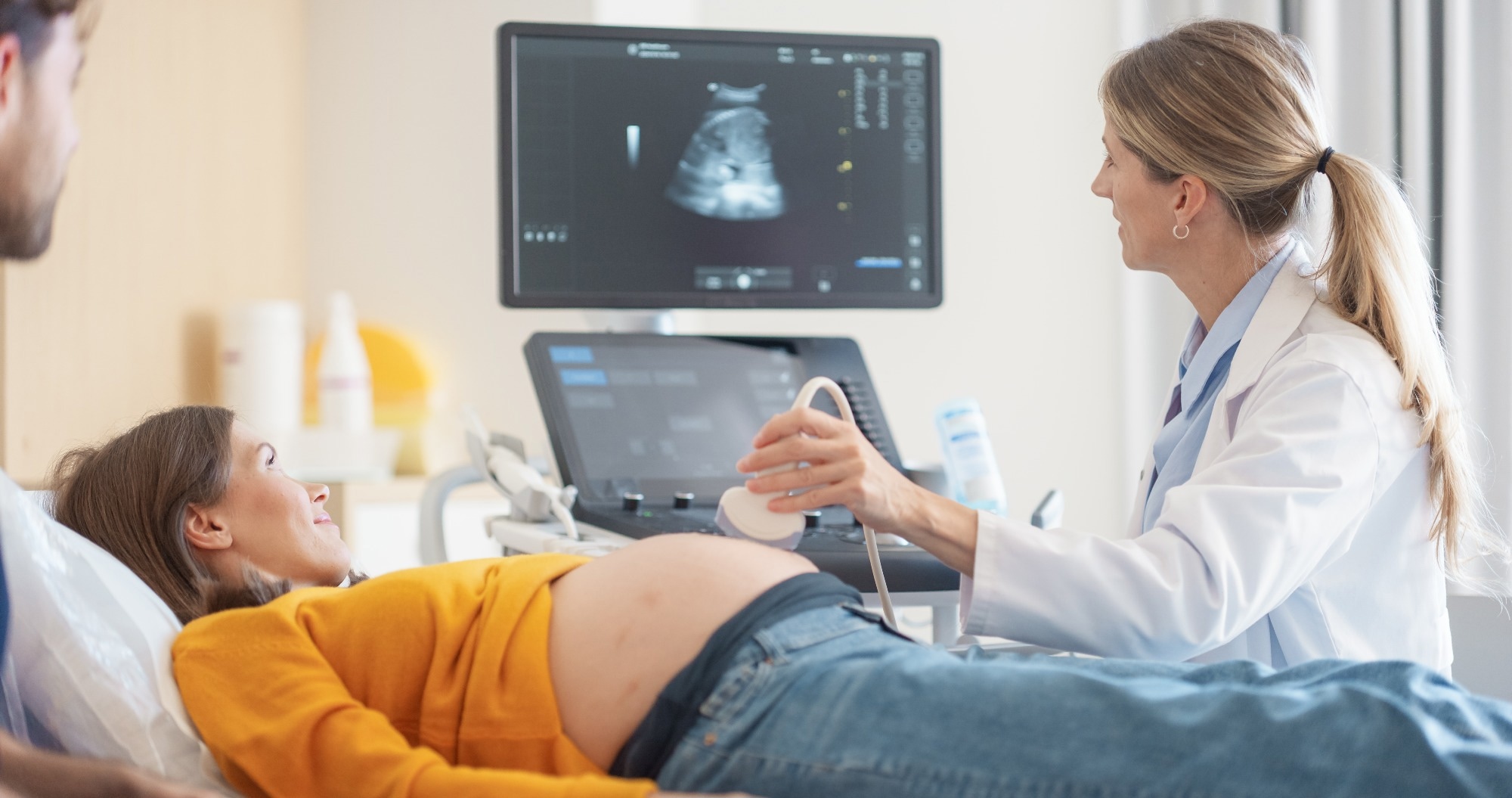
Research: Physician work patterns during pregnancy, parental leave, and return to work. Image credit: Gorodenkoff / Shutterstock
In a recent study published in JAMA network openresearchers examined physicians’ work patterns before, during, and after pregnancy.
Background of workload and vacation for pregnant doctors
Despite predictions that women will make up approximately 50 per cent of Canada’s physician workforce by 2030, pregnancy and parental leave in medicine is not well supported in medical culture. Parental leave may improve parents’ mental health and lead to longer breastfeeding periods. Given the lack of support and policies for working physicians to reduce maternity leave and overtime, pregnant physicians often maintain high workloads and take short parental leave.
Even after returning to work, doctors face discrimination from mothers and have limited breastfeeding facilities. Additionally, reduced income during leave can contribute to dissatisfaction and can pose significant problems for new physicians with loans. The additional burden placed on colleagues while on vacation also remains a major concern for physicians. Therefore, understanding leave patterns is important for planning the physician workforce, especially since leave needs to be envisioned as part of a sustainable healthcare workforce.
Ontario Physician Pregnancy Study Design
In the current study, researchers examined physicians’ work patterns before, during, and after pregnancy. Data from a licensed agency in Ontario, Canada, was used to identify deliveries at >20 weeks of gestation among practicing physicians from April 2002 to November 2018. Bills submitted by physicians to the Ontario Health Insurance Plan were used to determine work activity levels and work stoppages and resumptions. The doctors were followed until November 2023, allowing researchers to assess return-to-work patterns over time.
Physicians who submitted a claim within 2 years before pregnancy were included. The cohort was stratified into eight groups according to specialty: diagnostic imaging, psychiatry, obstetrics and gynecology, emergency medicine or anesthesiology, pediatrics, surgery, family medicine, and medical specialties. Claims were assessed for each trimester during the period from pregnancy to delivery.
Researchers assessed labor activity before and during pregnancy. Overall workload (24 hours) and nighttime workload (midnight to 7 a.m.) were assessed. In addition, no complaints after giving birth indicate leave, and 10 or more complaints within a week indicates return to work. Day and night labor rates before and during pregnancy were calculated per 100 person-days. The pre-pregnancy comparison period matches the same calendar period of the previous year, which helps account for seasonal variations in work patterns.
Work rate ratios were calculated for each semester using a negative binomial regression model. Additionally, we estimated the proportion of physicians returning to work and the time it took them to return to work. We calculated the cumulative probabilities of returning to work at 180 and 365 days postpartum by era (2002–2009 and 2010 and beyond) for each specialty group.
Work load and professional findings during pregnancy
A total of 5,948 births were confirmed among 3,932 physicians, and the median age at birth was 35 years. Approximately 80% of births were first or second births, and the remainder were third or higher. The median time from employee hire to pregnancy was 3.6 years. Most births occurred in family medicine groups (59%), followed by medical specialties (13.2%).
For the preconception period of interest, the median overall workload across specialty groups ranged from 44 to 67 days. In almost all specialties, it increased or remained stable in the first and second trimesters, but decreased in the third trimester. A similar trend was observed for night work activities with workloads ranging from 0 to 9 days. Across the cohort, work ratios increased during pregnancy compared to before pregnancy.
Compared to pre-pregnancy, the overall work rate increased in the first two trimesters but decreased in the third trimester. In particular, the overall duty ratios for third-trimester medical departments, obstetrics and gynecology, and diagnostic imaging groups were similar to pre-pregnancy levels. Night shifts decreased overall throughout pregnancy, except for the diagnostic imaging and psychiatry groups, which increased slightly during the first two trimesters of pregnancy and then decreased during the third trimester.
Night shift rates increased in all trimesters in the psychiatry group, but remained stable throughout pregnancy in the diagnostic imaging group. However, the authors noted that the absolute rate of night shifts in psychiatry is very low, which is important in interpreting this increase. High return-to-work rates were achieved across all specialty groups. Surgeons were the fastest to return to work (133 days) and psychiatrists were the slowest (270 days). The cumulative probability of returning to work by 180 days was 47.2% from 2002 to 2009 and 39.6% from 2010 onwards. We were able to compare both eras on a 365-day basis.
Parental leave and its impact on workforce equity
In summary, the workload of Ontario physicians increases during the first two trimesters of pregnancy, potentially leading to work being brought forward before the holidays. The authors suggested that this pattern may reflect financial pressures, group practice obligations, or a perceived need to offset the burden placed on colleagues during the holidays. Parental leave varied and was significantly shorter than that of Canadians receiving parental leave benefits.
This study has some limitations. Leave patterns among residents, male physicians, and physicians who became parents through adoption or surrogacy have not been evaluated. Local workplace policies, practice group arrangements, and the potential impact of the COVID-19 pandemic on leave periods have also not been assessed. Ensuring fair and appropriate parental leave is essential to promoting gender equality in healthcare and supporting workforce planning and physician retention.
Reference magazines:
- Simpson AN, Sutradar R, MacArthur E, Cushimano MC, Tanuseptro P, Baxter NN (2026). Physician work patterns during pregnancy, parental leave, and return to work. JAMA Network Open, 9(4), e267543. Doi: 10.1001/jamanetworkopen.2026.7543, https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2848014