For the first time since 2018, the American College of Cardiology and the American Heart Association have released updated clinical guidance on how to screen and manage blood cholesterol. The recommendations are: Journal of the American College of Cardiology and circulation The findings were presented March 28 at the American College of Cardiology’s 75th Annual Scientific Sessions in New Orleans.
The release came just before the companion paper, “The ABCs of cardiovascular disease prevention: Telling what we know in 2026,” was published in the journal. American Journal of Preventive Cardiology.
Focus on LDL, lipids and individual risks
The latest guidance focuses on lowering low-density lipoprotein (LDL) cholesterol, commonly known as bad cholesterol, and other blood fats such as lipoprotein(a) or Lp(a). It also highlights the need for early screening, especially for people with a family history of heart disease, and calls for a more individualized risk assessment based on factors such as pre-existing health conditions. These steps are intended to support more informed and shared decisions between patients and clinicians.
“We know that lower LDL cholesterol levels are better for reducing the risk of heart attack, stroke, and congestive heart failure,” says Roger S. Blumenthal, M.D., chair of the guideline committee and director of the Johns Hopkins Siccarone Center for Cardiovascular Disease Prevention. “We also know that lowering elevated lipids and blood pressure in young adults supports optimal heart and vascular health throughout life.”
Why early screening is important
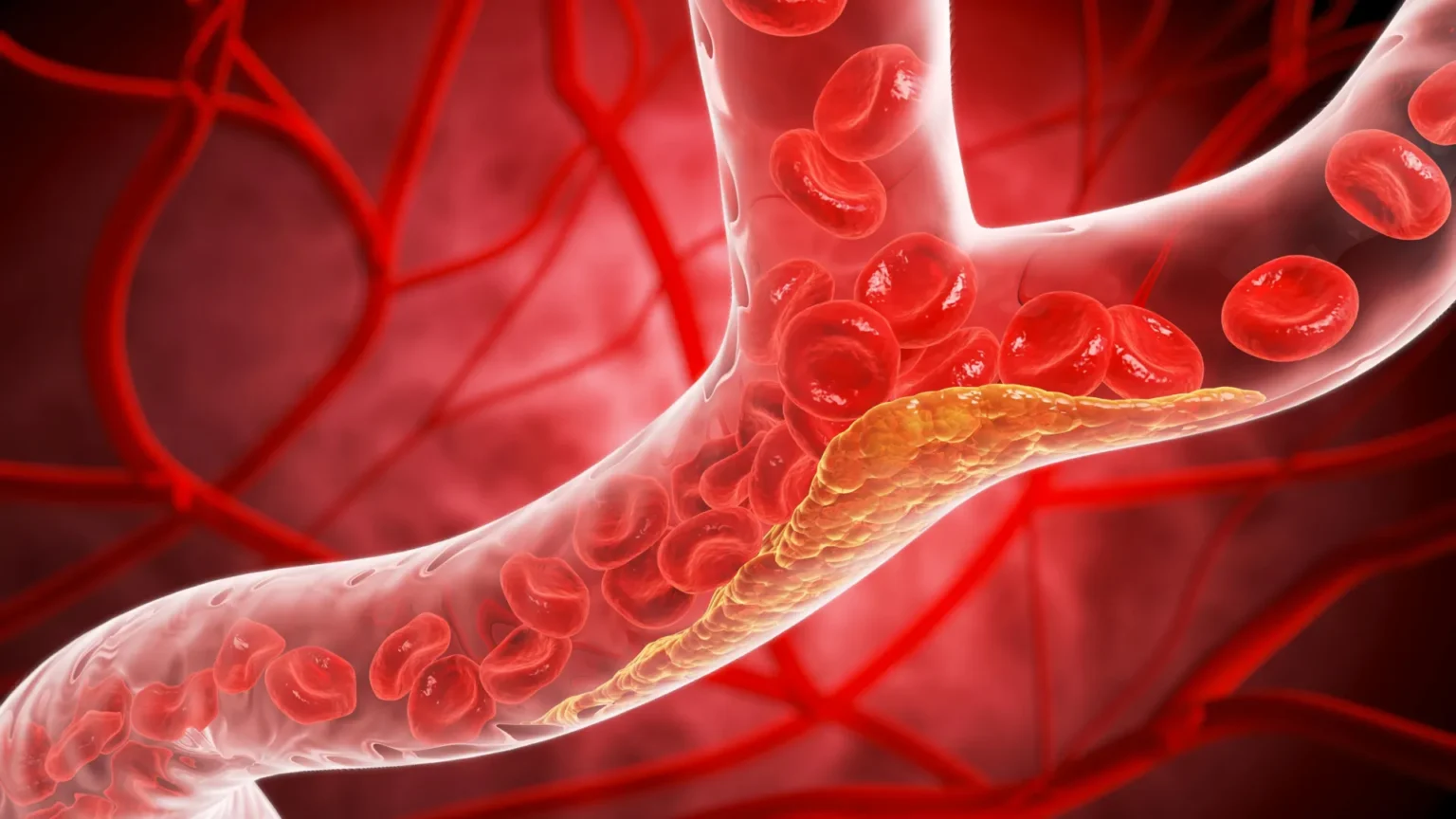
The latest information comes as studies show that about one in four adults in the United States has elevated LDL cholesterol (LDL-C), the main cause of atherosclerosis (narrowing or hardening of the arteries). A buildup of certain lipids can cause plaque to form on the inside of artery walls. This plaque can restrict blood flow and under certain conditions can rupture, causing a heart attack or stroke, or requiring emergency treatment to restore circulation.
Despite these risks, the core advice for maintaining heart health remains the same. Experts continue to emphasize the importance of eating a balanced diet, regular physical activity, avoiding smoking, getting enough sleep, and maintaining a healthy weight. According to Blumenthal, approximately 80% to 90% of cardiovascular disease is related, at least in part, to factors that people can modify, and lifestyle changes are an important first step.
Early screening and genetic risk factors
Key changes in the new guidelines include promoting testing at younger ages and considering individual risk more broadly. Physicians are encouraged to consider family history of atherosclerosis, underlying medical conditions such as rheumatoid arthritis, and life events such as early menopause and pregnancy complications such as preeclampsia and gestational diabetes when assessing risk and planning treatment.
For example, people with familial hypercholesterolemia, an inherited disease that causes very high LDL-C levels, currently need screening tests to begin around age 9 (or earlier). The guidance also recommends a single test for Lp(a). This is associated with genetic risk, with levels of 125 nanomoles per liter increasing the risk of heart disease by about 40%, and 250 nanomoles per liter potentially doubling the risk.
New risk calculator extends long-term forecasting
Another major update is the introduction of new tools to estimate 10- and 30-year heart attack and stroke risks. Previous models primarily focused on the 10-year risk for adults over 40 and relied on basic factors such as age, cholesterol levels, and blood pressure.
A new computational tool, Prediction of Risk of Cardiovascular Disease Events (PREVENT), includes additional measurements such as blood sugar levels and kidney function. It is designed to be used from the age of 30 and is based on data from 6.6 million people (compared to just 26,000 in the previous model).
“Shifting the paradigm toward aggressive prevention strategies early in life can meaningfully change the trajectory of cardiovascular disease and lead to improved health outcomes for people decades later,” says MHS’s Seth Martin, M.D., a cardiologist and member of the guideline development committee.
Additional testing and individualized treatment decisions
To further refine the risk estimate, the guidelines outline additional factors called “risk enhancers” that physicians may consider. For people with borderline or moderate risk, clinicians may use additional tests to guide decisions. These include measuring inflammation with high-sensitivity C-reactive protein (hsCRP), assessing Lp(a) levels, and considering family history and ancestry.
Imaging tools, such as a coronary calcium scan, are also recommended to detect calcium deposits that signal plaque buildup and can help tailor your treatment plan more precisely.
Expanding treatment options and lowering LDL targets
The latest guidance addresses treatment strategies for a wide range of groups, including people who are pregnant or breastfeeding, adults over 75, and people with conditions such as diabetes, advanced kidney disease, HIV, and cancer.
In addition to statins, the guidelines also include updated recommendations for other cholesterol-lowering therapies, including ezetimibe, bempedoic acid, and injectable PCSK9 monoclonal antibodies. These options are especially important for people who do not respond well to statins or who require multiple treatments to reduce LDL-C.
For people without cardiovascular disease, an LDL-C level of less than 100 mg/dL is considered optimal. Those at moderate risk are encouraged to lower their levels to below 70 mg/dL, while those at high risk should aim for below 55 mg/dL. The guidelines also include goals for non-HDL cholesterol and apolipoprotein B.
For the future
In an accompanying editorial, the experts suggest that future recommendations may place greater emphasis on lowering LDL-C to less than 55 mg/dL for patients with moderate atherosclerosis. This direction is supported by the results of the VESALIUS-CV clinical trial, which demonstrated the benefits of aggressively lowering cholesterol using a combination of treatments.
The 2026 Guidelines for the Management of Dyslipidemia were developed by the American College of Cardiology and the American Heart Association in collaboration with multiple healthcare organizations focused on cardiovascular health, prevention, and patient care.