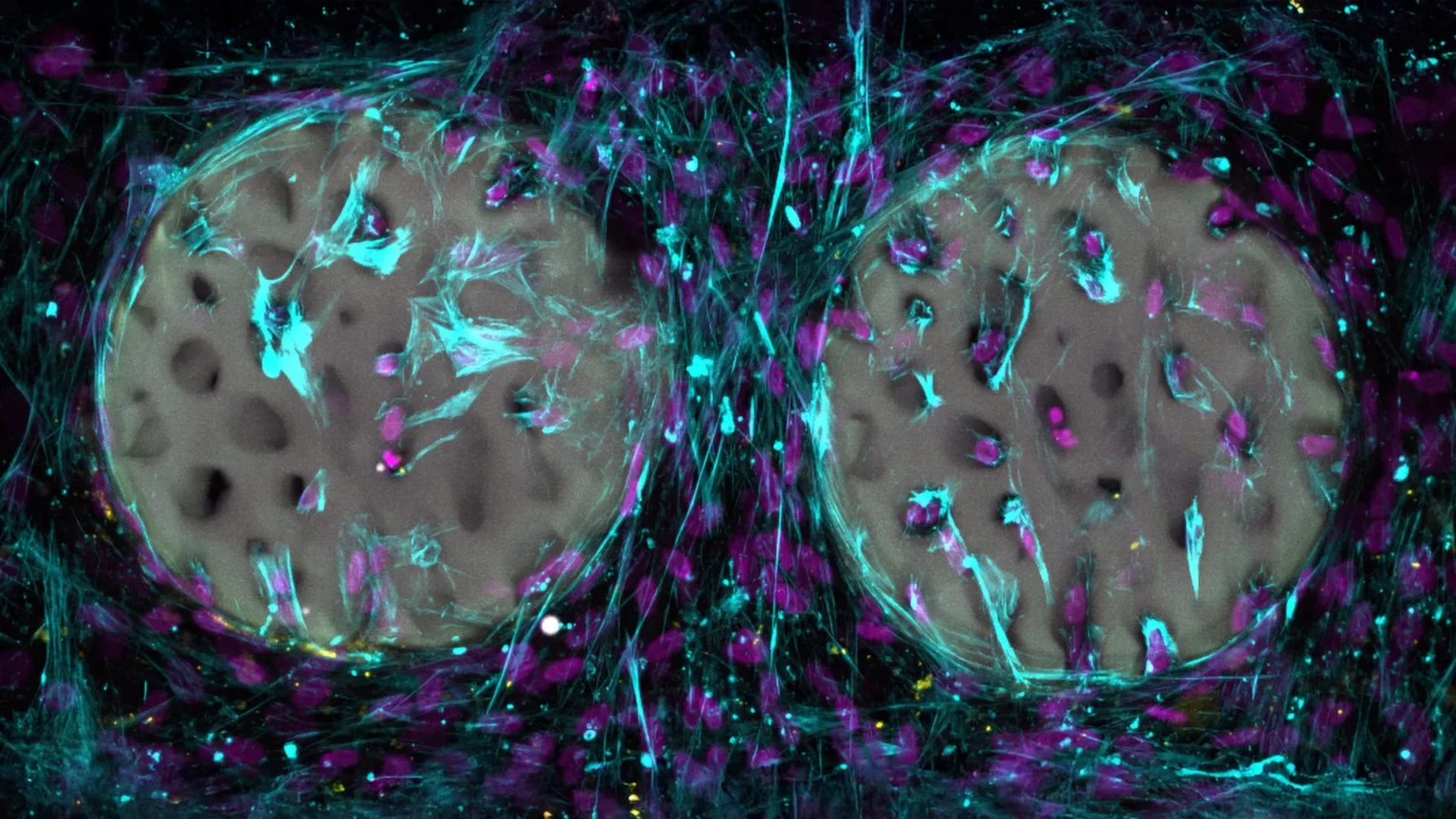
Bones fractured in (skiing) accidents often repair without medical intervention. However, if the fracture is particularly severe or a bone tumor needs to be surgically removed, doctors will rely on implants to stabilize the area and support new bone growth.
Today’s implants are typically made from the patient’s own bone, called an autograft, or from metal or ceramic materials. Autografts require additional surgery to harvest bone tissue, which increases recovery time and surgical risks. Problems can arise because metal implants are much harder than natural bone and can loosen over time, reducing long-term stability.
Biologically compatible bone implant design
Bones are much more complex than they appear. It contains countless microscopic tunnels and cavities that are essential for strength and function. “For proper healing, it is essential to incorporate biology into the repair process,” says Xiao Hua Qing, professor of biomaterials engineering at ETH Zurich. Successful bone repair depends on multiple cell types first migrating into the implant and then working together to build new tissue.
To better adapt to this biological complexity, Hata and his team, together with ETH professor Ralf Müller, developed a new type of hydrogel designed for future bone implants. The soft material, which has a jelly-like texture, gradually dissolves in the body and could eventually allow for customized implants for individual patients. Their discovery recently advanced materials.
Inspired by the body’s natural healing process
When a bone first breaks, the body does not immediately form hard tissue. Instead, it forms a soft and permeable structure. Early after injury, hematoma and bruising develop at the fracture site. This temporary scaffold allows immune and repair cells to move while delivering nutrients. A fibrin network connects these cells. Over time, this flexible framework slowly transforms into solid bone.
Newly developed hydrogels are designed to mimic this early healing phase. It is composed of 97% water and 3% biocompatible polymer. To control when and where it hardens, the researchers added two special molecules. One connects the polymer chains and the other reacts when exposed to light, causing the solidification process.
Qin and Muller’s former doctoral student Wangwan Qiu created a linking molecule specifically for this purpose. “This allows rapid structuring of hydrogels in the submicrometer range,” she says. When a laser pulse of a specific wavelength hits the material, the polymer chains instantly bond together to form a solid structure. Areas that are not exposed to the laser remain soft and can be removed later.
Record-breaking laser printing at the nanoscale
Using this technique, the team is able to precisely shape highly detailed hydrogels. Lasers can create structures as small as 500 nanometers.
“Hydrogels are difficult to mold because they resemble jelly,” says ETH’s Professor Qin. “Using our newly developed connecting molecules, we are not only able to structure hydrogels in a stable and extremely fine-grained way, but we are also able to generate hydrogels with fast writing speeds of up to 400 millimeters per second, which is a new world record.”
In their experiments, the researchers created highly detailed hydrogel structures modeled after real bones. Using medical images as a guide, they recreated the delicate lattices known as trabeculae that give bones their internal strength.
Natural bone itself contains an amazing network of fluid-filled channels just nanometers wide. “The dice-sized bone fragment contains 74 kilometers of tunnels,” Hata said. For comparison, the world’s longest railway tunnel, the Gotthard Base Tunnel, is 54 kilometers long.
Early clinical tests show promising results
So far, this material has only been evaluated in laboratory experiments. In test tube studies, bone-forming cells quickly migrated into the structured hydrogel and began producing collagen, a key component of bone. The researchers also confirmed that the material is biocompatible and does not harm these cells. The material has been patented, and the research team plans to provide it to medical manufacturers.
The ultimate goal is to make hydrogel-based implants available for clinical use in fracture repair. Further research is still needed. Mr. Hata is preparing for animal experiments in partnership with the Davos AO Institute. These tests test whether the material supports the movement of bone-forming cells in vivo and restores bone strength over time.