Extensive human data reveals that even a single dose of antibiotics can leave a measurable microbial footprint years later, raising important questions about long-term health effects and prescribing practices.

Study: Linking antibiotic use and gut microbiome composition from individual-level prescription data for 14,979 people. Image credit: marevgenna / Shutterstock
In a recent study published in the journal natural medicineresearchers found that the effects of antibiotics on the gut microbiome can last much longer than expected. By linking Swedish prescription registry data with fecal metagenomic profiles from approximately 15,000 adults across multiple population-based cohorts, this study shows that even a single dose of antibiotics four to eight years ago is associated with persistent differences in microbiome composition.
These findings highlight the potential for long-term disruption of the microbiome and emphasize the need to use antibiotics cautiously, as even routine prescriptions can have lasting health effects.
Disruption of the gut microbiome and risk of chronic disease
Disruption of the gut microbial ecosystem is increasingly recognized as a key contributor to a wide range of health conditions, including cardiometabolic diseases, autoimmune diseases, and colorectal cancer. Antibiotics are a major factor in causing these imbalances, and repeated or long-term use is associated with increased risk of obesity, type 2 diabetes, and cardiovascular disease.
Small intervention studies have shown that microbial diversity rapidly decreases and major bacterial groups change after treatment. However, these findings primarily reflect short-term effects. As antibiotic use remains widespread, understanding the long-term effects on gut microbial communities has become an important research priority, but robust large-scale evidence is limited.
Population study design and microbiome analysis methods
In this population-level study of 14,979 people, researchers examined the effect of oral antibiotic use over the past eight years on gut bacterial composition. They linked prescription data from the Swedish National Prescription Drug Register (NPDR) with fecal metagenomic data from three cohorts: the CARdioPulmonary bioImage Study (SCAPIS), the Swedish Infrastructure for Medical Population-based Life-course and Environmental Research (SIMPLER), and the Malmö Offspring Study (MOS).
The researchers assessed antibiotic exposure over three time periods: within 1 year, within 1 to 4 years, and within 4 to 8 years before sampling. Patients with recent antibiotic use, inflammatory bowel disease, or chronic lung disease were excluded. Fecal samples were subjected to deep shotgun metagenomic sequencing, and microbial diversity was quantified using indices such as Shannon index and inverse Simpson index. Taxonomic classification was performed using the Genomic Classification Database.
Multivariate regression models assessed the association between antibiotic exposure and microbiome diversity, adjusting for confounders such as age, sex, body mass index (BMI), smoking status, education, and comorbidities. The model also considered drugs such as proton pump inhibitors (PPIs), statins, metformin, beta blockers, antipsychotics, and selective serotonin reuptake inhibitors (SSRIs).
Sensitivity analyzes tested alternative exclusion criteria, and spline-based models investigated microbiome recovery over time. Subgroup analyzes were performed by age and gender.
Persistent microbiome changes after antibiotic exposure
Antibiotic use was common, with approximately 70–74% of participants receiving at least one prescription in the past 8 years. Broad-spectrum penicillins, penicillin V, and tetracyclines were most frequently used.
The greatest reduction in microbial diversity occurred within 1 year of antibiotic use. However, significant associations persisted for exposures 1 to 4 years ago and then 4 to 8 years ago. Each additional course led to a further decline in diversity. Remarkably, even a single course taken years ago was associated with long-term differences in the microbiome.
Clindamycin, fluoroquinolones, and flucloxacillin showed the strongest and most durable effects. These antibiotics were associated with changes in the relative abundance of microbial species of up to approximately 10–15%. beneficial species such as common list and Odoribacter spruninix I declined. In contrast, species associated with metabolic risk include: Ruminococcus gnabus, Flavonifractorpurutiand eggerterra downhas increased in large quantities. The effect of penicillin V was relatively minimal.
Microbiome recovery was fastest during the first two years after antibiotic use, but was slower and often incomplete thereafter. Recovery varies by antibiotic type, gender, and age, suggesting that the resilience of the microbiome varies between individuals. Sensitivity analyzes confirmed the robustness of these results.
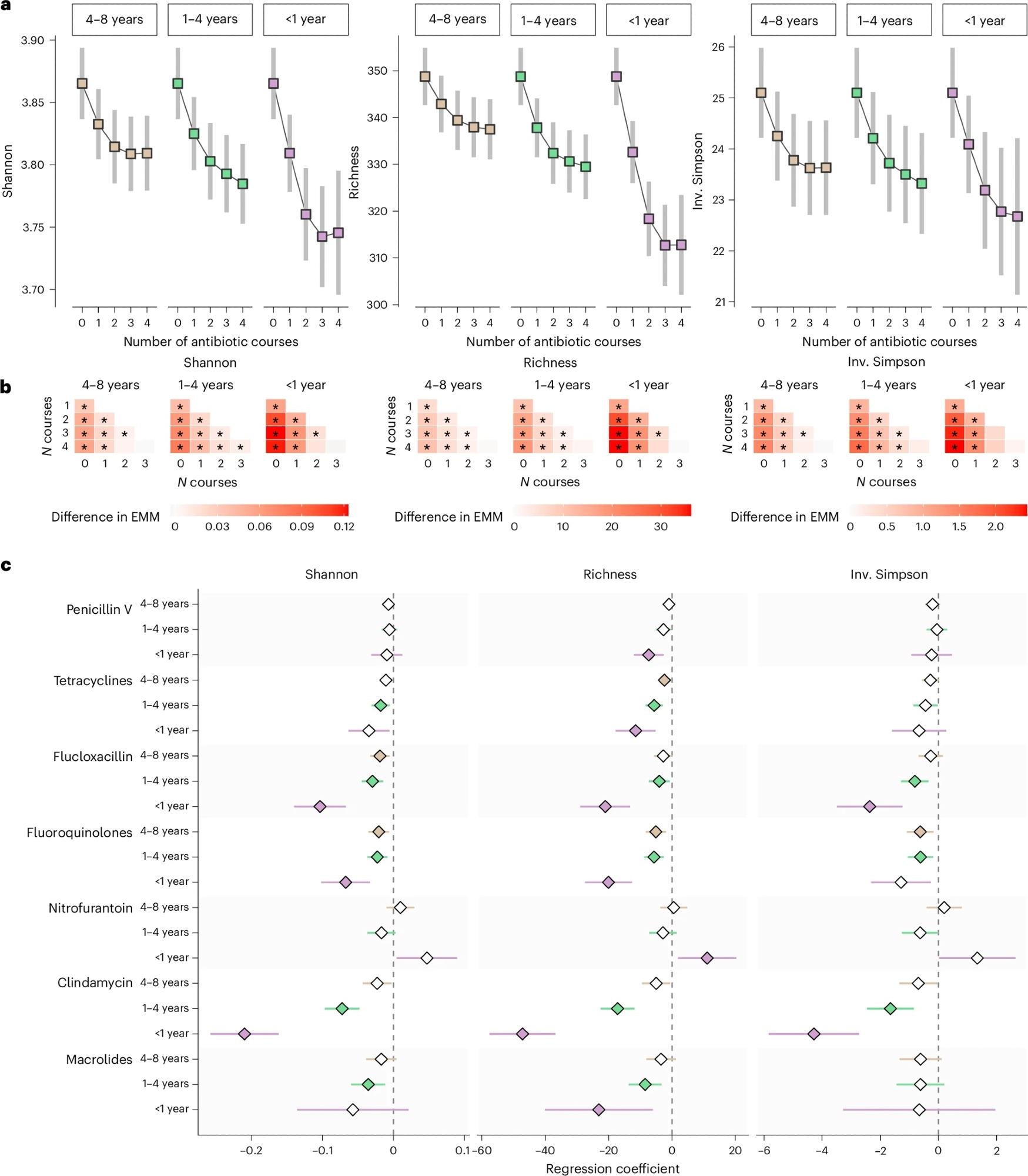
bemicrobiome diversity indicators (Shannon index, species richness and inverse (Inv.) Simpson index) for each additional course of antibiotics 4–8 years, 1–4 years and <1 year before fecal sampling. Estimated marginal means (EMMs) of diversity were obtained using regression models with antibiotic exposure modeled using restricted cubic splines and adjusting for age, sex, smoking, education, country of birth, site-specific analysis plate, BMI, Charlson Comorbidity Index, polypharmacy, PPIs, metformin, SSRIs, statins, beta-blockers, and antipsychotic use (n = 14,974). Squares represent EMMs and bars represent 95% confidence intervals. bEMM pairwise differences in microbiome diversity by number of previous antibiotic courses. Stars indicate significant differences (FDR < 5%). cThe association between antibiotic use during the 8 years before fecal sampling and gut microbiota species diversity was investigated in three cohorts (SAPIS, SIMPLER, MOS, total n = 14,974) using regression models adjusted for the same covariates as above, followed by a meta-analysis of regression coefficients. The x-axis and diamonds display meta-analyzed regression coefficients. Error bars represent 95% confidence intervals. Black symbols indicate statistically significant associations (FDR < 5%). At least one antibiotic has been shown to have such associations.
Implications for antibiotic stewardship and future research
The findings suggest that some antibiotics can have long-term effects on the gut microbiome that can persist for more than four years. These results support smarter antibiotic prescribing and management strategies that minimize microbiome disruption.
However, this study is observational and cannot prove cause and effect. Further research is needed to understand the long-term health effects, including associations with chronic diseases. The findings may not be generalizable beyond the Swedish outpatient setting, and total antibiotic exposure may be underestimated due to missing hospital or international prescribing data.
Reference magazines:
- Baldanzi, G. et al. (2026). Antibiotic use and gut microbiota composition were linked from individual-level prescription data for 14,979 individuals. Natural Medicine, 1-11. DOI: 10.1038/s41591-026-04284-y, https://www.nature.com/articles/s41591-026-04284-y


