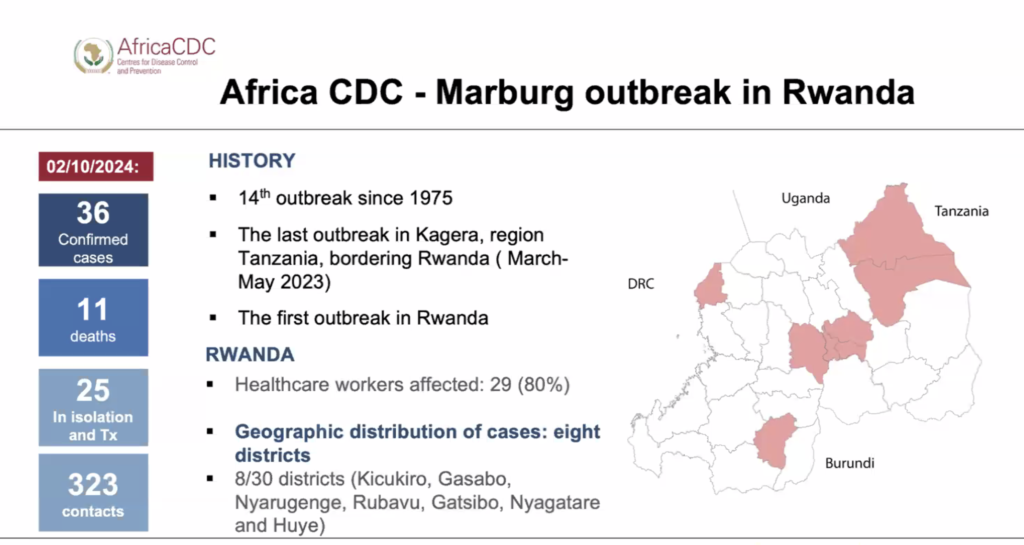
During the first Marburg virus outbreak in Rwanda, clinical evaluation was complicated by the fact that patients were also battling malaria. The Rwanda Biomedical Center (RBC) had diagnostic kits to confirm the infection, but additional genome sequencing was needed to investigate the source.
For complex cases involving multiple pathogens, metagenomic next-generation sequencing (mNGS) provides a more comprehensive approach. This advanced diagnostic capability is critical to saving time and improving patient outcomes during outbreaks.
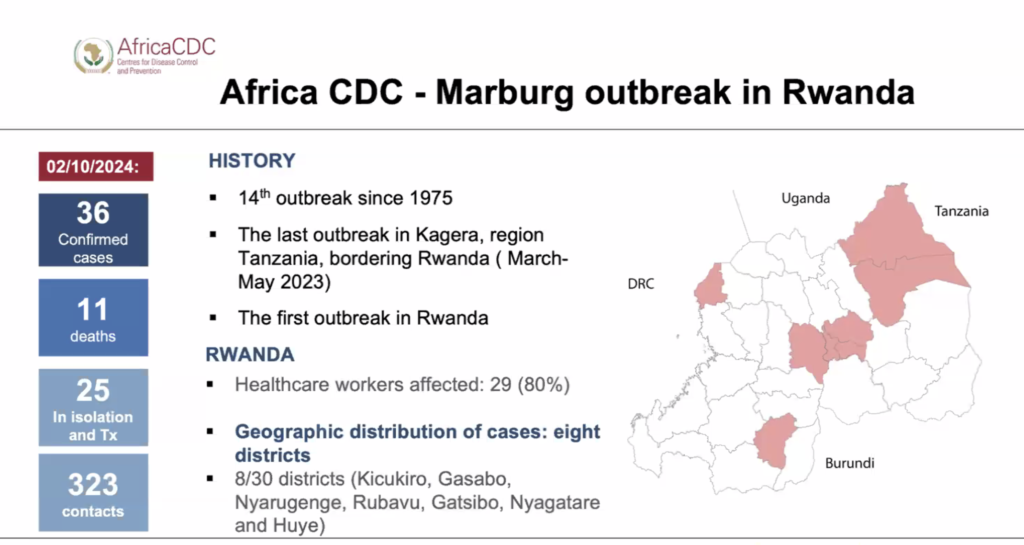
Image credit: AfricaCDC
The cost of inaction is $350 billion.
In a world of high-threat pathogens, delays are measured in both lives and GDP. The WHO says the case fatality rate for Marburg disease could rise to 88% if uncontrolled, and that the economic “epidemic” is also viral.
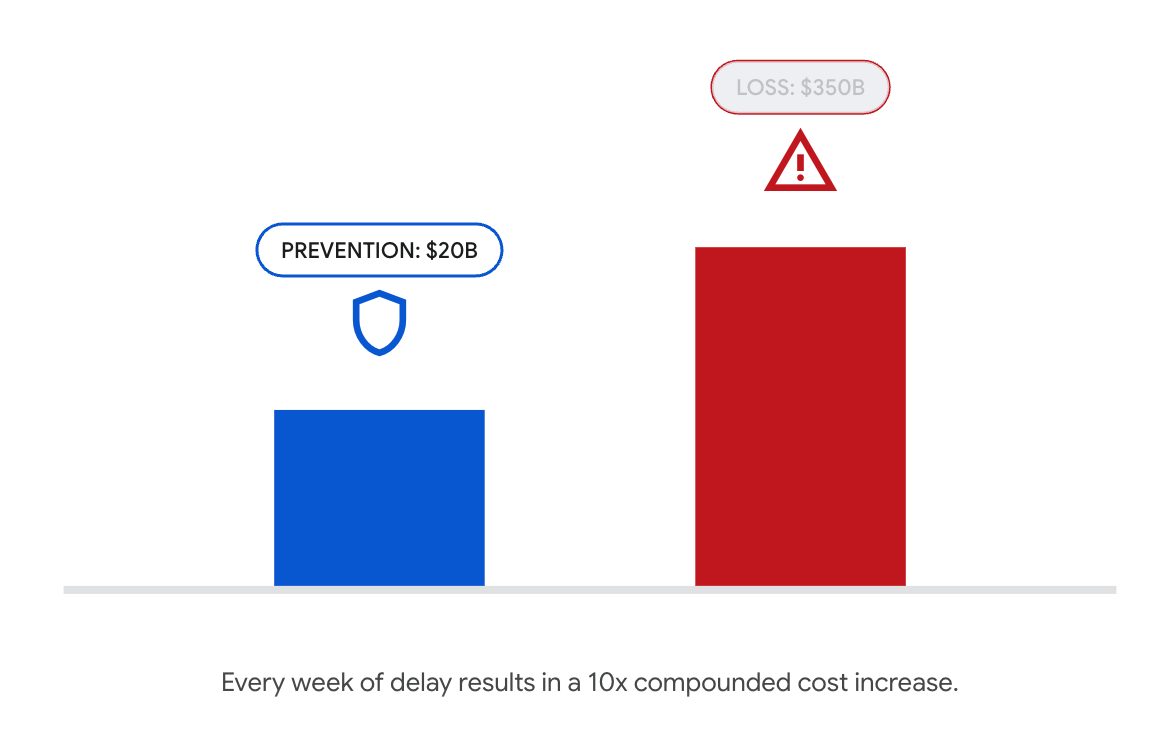
Image credit: AfricaCDC
A 2022 study suggests that economic damage could be 10 to 100 times greater if infectious disease control is delayed by just one week. Zoonotic disease inaction alone claims 3.3 million lives and costs more than US$350 billion annually. In contrast, effective global prevention is estimated to cost just US$20 billion annually.
“Ignorance of genomics-based research is a luxury that the global economy can no longer afford,” argues Dr. Atsubeha Gebregziabsiel Weldemariam of the Ethiopian Institute of Public Health. His team was working on the front lines of disease control by analyzing large numbers of samples.
Technical “blind spots”
Professor Claude Mambo Mvuni, director of the Rwanda Biomedical Center, warns that traditional killers such as malaria and tuberculosis are often overshadowed by new threats. Dengue fever, for example, often goes undetected, even though the global incidence has skyrocketed eightfold in 20 years.

Image credit: AfricaCDC
To break this cycle, Professor Mvuni advocates a paradigm shift towards molecular diagnostics. “Molecular assays can often detect pathogens with greater than 95% sensitivity before clinical complications occur,” he noted, adding that for high-threat infections like chikungunya and Nipah viruses, early detection is a key driver of improved outcomes. His advice to the public is clear. “High-precision diagnostics are becoming increasingly cost-effective when evaluated from the perspective of population health,” he said, and the prompt use of validated testing services.
2025 study shows that conventional tests miss dengue/typhoid fever (25-35% lower sensitivity) compared to advanced multidiagnostics to identify co-circulating pathogens. This reinforces the uncertainty of the “black box” and the stigma of isolation, driving patients away from the hospital. Clinicians then turn to broad-spectrum antibiotics ‘just in case’, which fail to treat viral infections while actively accelerating antimicrobial resistance (AMR) and exacerbating the impact of future epidemics.
BGI Genomics PMseq™ uses mNGS technology to support global efforts in the analysis and investigation of complex infectious disease cases and tailor effective treatments.
Precision as a pillar of health
When clinical symptoms alone are insufficient to identify rare or emerging threats, metagenomic next-generation sequencing (mNGS) offers a decisive advantage by providing unbiased and culture-independent detection of all microbial nucleic acids in a single sample.

Image credit: AfricaCDC
BGI Genomics’ PMseq™ is a sensitive solution that provides comprehensive DNA and RNA pathogen detection based on mNGS, supporting both individualized clinical diagnosis and large-scale biosurveillance. This early warning system played a central role in the initial identification of SARS-CoV-2 and the novel Bunyavirus, and has already demonstrated real-world impact.
By leveraging vast reference databases and advanced bioinformatics, the platform characterizes pathogens in near real-time and identifies threats, often before they are fully recognized by the global health community.
China and Africa precision cooperation
The transition to “scientific management” is increasingly defined by local high-tech precision. An important pillar of this is evolving advanced medical collaboration.
Professor Muvunyi points out that partners like BGI Genomics are moving towards a co-development model. “Evidence shows that countries with local genomic capacity can respond to outbreaks up to three times faster than countries that rely on external assistance,” he says. “Co-ownership of innovation is key.”

Dr. Atsubeha presented the certificate of accreditation at the China CDC and Africa CDC workshops. Image credit: AfricaCDC
During a high-level communication at the Africa Centers for Disease Control (CDC) in late 2025, Chinese health experts conducted intensive training on genome sequencing. Dr. Atsubeha witnessed that automated extraction technology introduced by Chinese experts allows health professionals in Africa to isolate bacteriophages within 20 minutes, allowing for a much faster response in the event of an outbreak.

Image credit: AfricaCDC
“The takeaway from this training is clear: African genomics facilities need to move from manual processes that take weeks to automated Chinese DNA sequencing technology capable of near real-time analysis,” he recalled.
balanced progress
Achieving true resiliency requires more than just hardware. It requires a science-driven response that replaces fears of “black box” isolation with community-led support.
By combining automated tools with a locally empowered workforce, health systems can ensure that when the next “diagnostic knot” emerges, the ability to untie it is already held in local hands.
About BGI Genomics
Headquartered in Shenzhen, China, BGI Genomics is the world’s leading integrated solutions provider for precision medicine. Our services cover more than 100 countries and territories and involve more than 2,300 healthcare institutions. In July 2017, as a subsidiary of BGI Group, BGI Genomics (300676.SZ) was officially listed on the Shenzhen Stock Exchange.