New research reveals that attention-deficit/hyperactivity disorder actually consists of at least two distinct brain structural subtypes, each with unique physical characteristics and behavioral symptoms. These structural differences suggest that patients may ultimately benefit from highly individualized diagnostic and therapeutic strategies based on their unique biology. The study was published in the journal General psychiatry.
Attention-deficit/hyperactivity disorder is a highly common neurodevelopmental disorder that affects children and adolescents around the world. Patients typically exhibit a variety of symptoms that fall into categories such as inattention, hyperactivity, and impulsivity. Because the symptoms vary from child to child, medical professionals classify the symptoms into several clinical manifestations based on these overlapping behaviors.
To understand the physical causes of symptoms, researchers often use magnetic resonance imaging, commonly known as MRI, to examine the structure of the brain. This non-invasive technology uses powerful magnets and radio waves to create detailed three-dimensional images of the central nervous system. Scientists use these images specifically to examine gray matter, the dark tissue in the brain that contains the main cell bodies of neurons.
Gray matter acts as the main processing center of the human brain. Responsible for routing sensory information, controlling voluntary movements, and managing complex functions such as memory and emotion. This important organizational structural change can significantly alter a person’s cognitive abilities and daily behavior.
Scientists studying this disorder often look for structural changes in specific brain regions, such as the prefrontal cortex, amygdala, and hippocampus. The prefrontal cortex handles executive functions such as planning, decision making, and impulse control. The amygdala and hippocampus are deeply involved in emotional regulation, memory storage, and reward processing.
In the past, brain imaging studies on this disorder have yielded highly inconsistent results. When researchers compared the brain scans of children with the condition with those of typically developing children, physical differences often blurred or appeared contradictory.
Tianzheng Zhong, a researcher at China’s Shandong First Medical University, wanted to understand the reasons behind these different results. Zhong and his colleagues suspected that existing clinical categories did not fully capture the physical differences in patients’ brains. They hypothesized that the condition contains hidden physical subtypes that correspond to different patterns of structural brain changes.
To test this idea, Zhong and his research team analyzed structural MRI data from a large public database. They rigorously filtered the information to exclude poor quality scans and incomplete clinical records. Their final sample included 135 children and adolescents diagnosed with the condition and 182 neurotypical youth who served as a control group.
First, the researchers directly compared the overall gray matter of all diagnosed patients to a neurotypical control group. In this broad comparison, differences in gray matter were not statistically significant. The research team noted that due to the diverse physical manifestations of the condition, opposing structural changes are likely to cancel each other out during analysis.
To overcome this hurdle, the team used advanced machine learning algorithms to group patients purely based on their brain anatomy. This computational tool sorts through large amounts of anatomical data to find hidden biological patterns that human observers might miss. The algorithm successfully identified two separate physical subtypes hidden within the patient group.
Once patients were classified into these two categories, distinct physical and behavioral patterns emerged. Researchers found that previously contradictory data began to make sense when viewed through the lens of these new groupings. Each subtype showed unique characteristics of brain volume changes and behavioral trends.
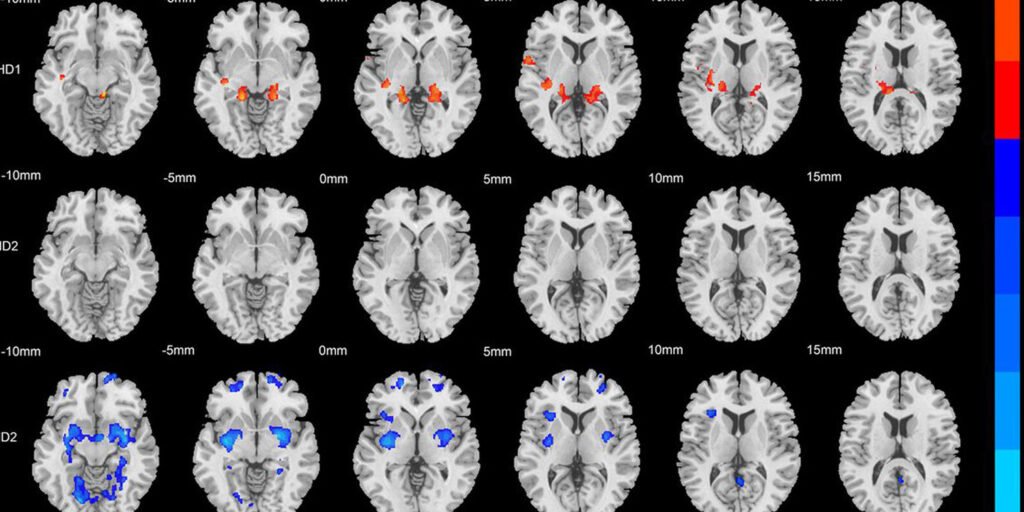
The first subtype was characterized by increased gray matter across several regions of the brain. Upon closer examination, the researchers found that these physical increases were concentrated in the frontal region and cerebellum. The frontal region handles higher cognitive functions such as working memory, and the cerebellum manages attention and motor coordination.
Behaviorally, patients in this first subtype suffered the most from severe inattention. The researchers noted that structural changes in this group were strongly related to an inability to maintain concentration. The physical growth of these specific brain areas appears to directly impact a patient’s attention span.
The second subtype showed almost the opposite physical reality. This group of patients showed extensive reduction or atrophy of gray matter compared to the neurotypical control group. This tissue loss was particularly pronounced in the bilateral cerebellum, frontal regions, and hippocampus.
The hippocampus is a specialized brain structure deeply involved in memory formation, spatial cognition, and internal motivation. In this second subtype, structural deterioration in these regions was associated with increased overall disease severity. These patients exhibited both symptoms of inattention and highly hyperactive or impulsive behavior.
After establishing these two subtypes, the researchers wanted to investigate how these brain changes progress as symptoms worsen. Since it is not possible to follow the same children over many years, they used mathematical methods to simulate the timeline of the disease. They organized the brain scans by severity of symptoms, from mild to severe, creating a pseudo-time series.
By arranging the data in this way, the team was able to perform causal network analysis. This statistical method helps identify brain regions that are causing physical changes associated with specific symptoms. They investigated how changes in one brain region reliably predict changes in another when symptoms worsen.
For the first subtype, this progressive analysis showed strong associations between specific brain nodes and inattentive behavioral regions. The data showed that attentional dysfunction was the main biological impairment for these children. Frontal regions and the cerebellum served as major hubs for these cascading structural changes.
In the second subtype, causal network analysis revealed broader patterns of structural connections. Physical changes in these children were caused by multiple behavioral areas, including severe hyperactivity and impulsivity. This widespread pattern reflects the overall increasing severity of the second group of conditions, with the hippocampus acting as a major hub.
Although the study provides a new way to categorize symptoms, the researchers noted some limitations to their approach. The data they used was cross-sectional. In other words, it provided only one snapshot of each child’s brain at a given moment. The simulated timeline based on symptom severity may not fully capture how the disorder naturally develops as the child ages.
Future studies will need to follow the same group of children over several years to confirm these patterns of progression. Long-term studies will allow scientists to observe these structural changes in the brain in real time. Observing brain growth and change is essential to fully understand the state of neurodevelopment.
If verified in future studies, these findings could ultimately change the way doctors diagnose and treat patients. Currently, this disorder is often treated with a one-size-fits-all approach, but these different physical subtypes suggest that individualized interventions may be highly effective. Understanding children’s unique brain structures may help doctors choose the most appropriate treatment.
Patients in the first subtype are likely to benefit most from targeted cognitive training designed to strengthen their attention networks. Their main symptom is inattention, so treatment that focuses on building working memory and concentration can be very beneficial. This approach directly addresses the biological mechanisms operating in specific brain subtypes.
Alternatively, patients in the second subtype may require an entirely different approach to disease management. Because they experience extensive gray matter loss and higher overall severity, they may require a more intensive combination of pharmacotherapy and behavioral therapy. Tailoring treatments to these different neuroanatomical profiles could pave the way to a new era of precision medicine in psychiatry.
The study, “Brain Morphological Changes Across the Behavioral Spectrum in Attention Deficit/Hyperactivity Disorder,” was authored by Tianzheng Zhong, Feng Wang, Jianfeng Qiu, and Weizhao Lu. Provides a new perspective on the biological basis of neurodevelopmental disorders.