A new review suggests that vitamin D does more than support bones in childhood, but says more solid human evidence is still needed for its most powerful non-skeletal effects.
Important points
Vitamin D is clearly important for skeletal health during the first 1,000 days, especially for preventing rickets and supporting early bone development.
This review suggests that vitamin D may also influence immune, metabolic, and selected neurodevelopmental pathways, providing biological plausibility as a programming factor in early childhood.
Most evidence for non-skeletal benefits in humans remains complex, limited and context-dependent, with stronger signals often observed in people and populations with vitamin D deficiency.
The authors argue that future research should move toward more individualized supplementation strategies, including consideration of genetics, baseline vitamin D status, and timing of exposure during pregnancy and childhood.
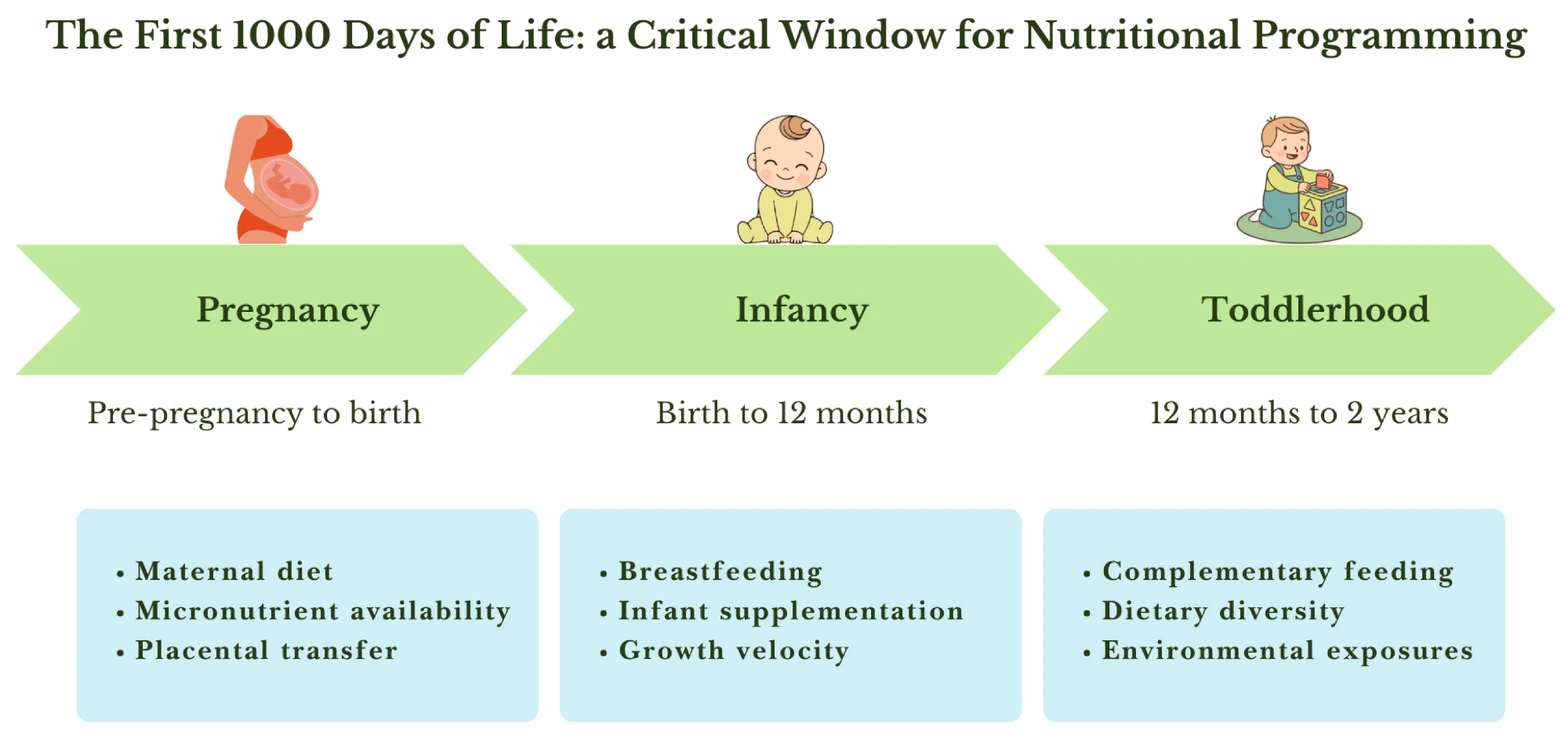
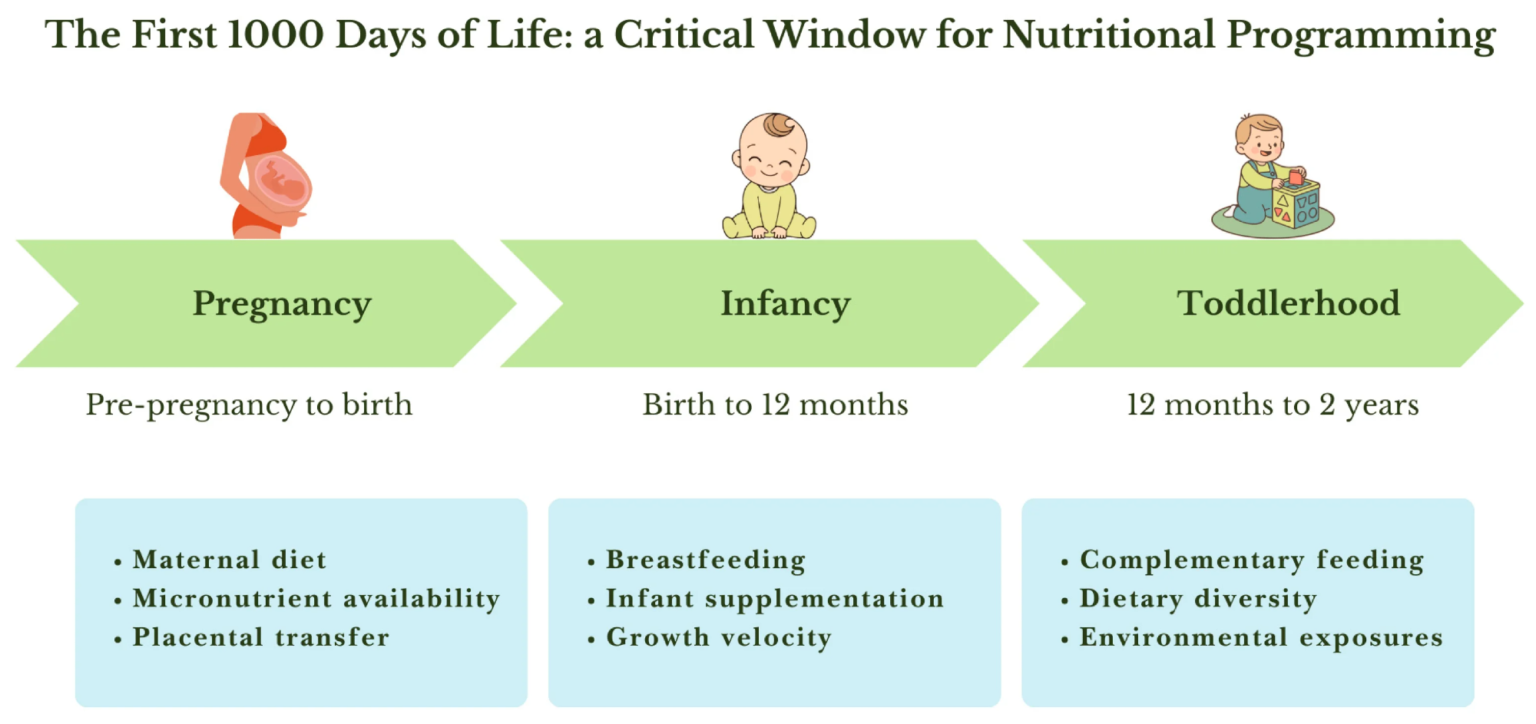
Key maternal, infant, and environmental factors that influence nutrition programs during pregnancy, infancy, and early childhood.
In a recent review published in a magazine nutrientsResearchers leveraged the Origins of Health and Disease (DOHaD) framework to assess the physiological role of vitamin D (vitD) during the first 1,000 days of human life.
This review reveals that early vitD is essential for nutritional prevention of skeletal diseases such as rickets. More importantly, this review highlights emerging data showing that vitamin D affects more than 1,000 genes through the nuclear vitamin D receptor (VDR) and may be associated with immune, metabolic, and selected neurodevelopmental health.
This review concludes that although vitamin D shows biological plausibility as a programming factor, current human clinical evidence for non-skeletal outcomes is early and incomplete, leading to heterogeneous and context-dependent findings.
background
The first 1,000 days of a newborn’s life are now considered both a “window of opportunity” and a “window of susceptibility” in pediatric practice, during which environmental stimuli significantly determine long-term health trajectories. Vitamin D, also known as the “sunshine vitamin,” has been historically studied for its role in calcium phosphate homeostasis.
More recent studies have shown that vitamin D has significant extraskeletal effects. Despite its important role, vitamin D deficiency remains a global health concern, estimated to affect approximately 28% of the population.
A meta-analysis of pregnant populations (n > 54,000) found that this group was particularly susceptible to vitamin D deficiency, with 54% having serum 25(OH)D levels below 20 ng/mL (50 nmol/L). Because neonatal storage is highly dependent on maternal transplantation, maternal deficiency may predispose the infant to adverse outcomes.
About reviews
The present narrative review aimed to address this knowledge gap by synthesizing recent literature examining the effects of vitamin D across pregnancy, infancy, infancy, and early childhood. Studies were identified from the PubMed, Scopus, and Cochrane databases and included systematic reviews, meta-analyses, randomized controlled trials (RCTs), and high-quality observational studies.
Key outcomes investigated include biomarkers such as serum 25(OH)D concentrations, skeletal outcomes such as bone mineral content (BMC) and bone mineral density (BMD), immune and metabolic indicators such as acute respiratory tract infection (ARTI) and body mass index (BMI), and molecular pathways such as transcriptomics and epigenetics.
The analysis also looked at different vitamin D dosing regimens, from a standard 400 IU/day supplement to a high-dose maternal intervention of 6,400 IU/day during breastfeeding.
Review the findings
Our findings reveal that vitD is involved in several physiological functions across developmental regions.
Regarding skeletal development, supplementation at 1,000 IU/day during pregnancy increased neonatal whole-body BMC with some persistence into mid-infancy, although the long-term clinical relevance remains unclear.
Regarding immunomodulation, a meta-analysis of more than 48,000 participants showed that vitamin D supplementation, specifically between 400 and 1,000 IU per day, slightly reduced ARTI risk. However, the effect was not significant in infants younger than 1 year, indicating an age-dependent response.
Regarding metabolic and birth outcomes, low maternal 25(OH)D levels are associated with higher risk of small for gestational age (SGA) infants and lower birth weight in observational studies of more than 35,000 mother-infant pairs, but randomized trial data remain inconsistent.
Regarding molecular programming, maternal nutritional supplementation was associated with decreased epigenetic gestational age acceleration and changes in placental gene expression, but the clinical significance remains unclear.
conclusion
This review supports the biological plausibility of vitamin D as a nutritional programming factor during early childhood. Its role extends beyond skeletal health to possible effects on immune tolerance and neurodevelopment, although evidence regarding these outcomes is still emerging and heterogeneous.
The 2024 Endocrine Society Guidelines empirically recommend approximately 2,500 IU of supplements per day during pregnancy, but emphasize that non-skeletal effects are still inconclusive.
Future studies should employ precision nutrition approaches that take into account genetic variations, including polymorphisms in vitamin D-binding protein (DBP), which may influence an individual’s response to supplements.