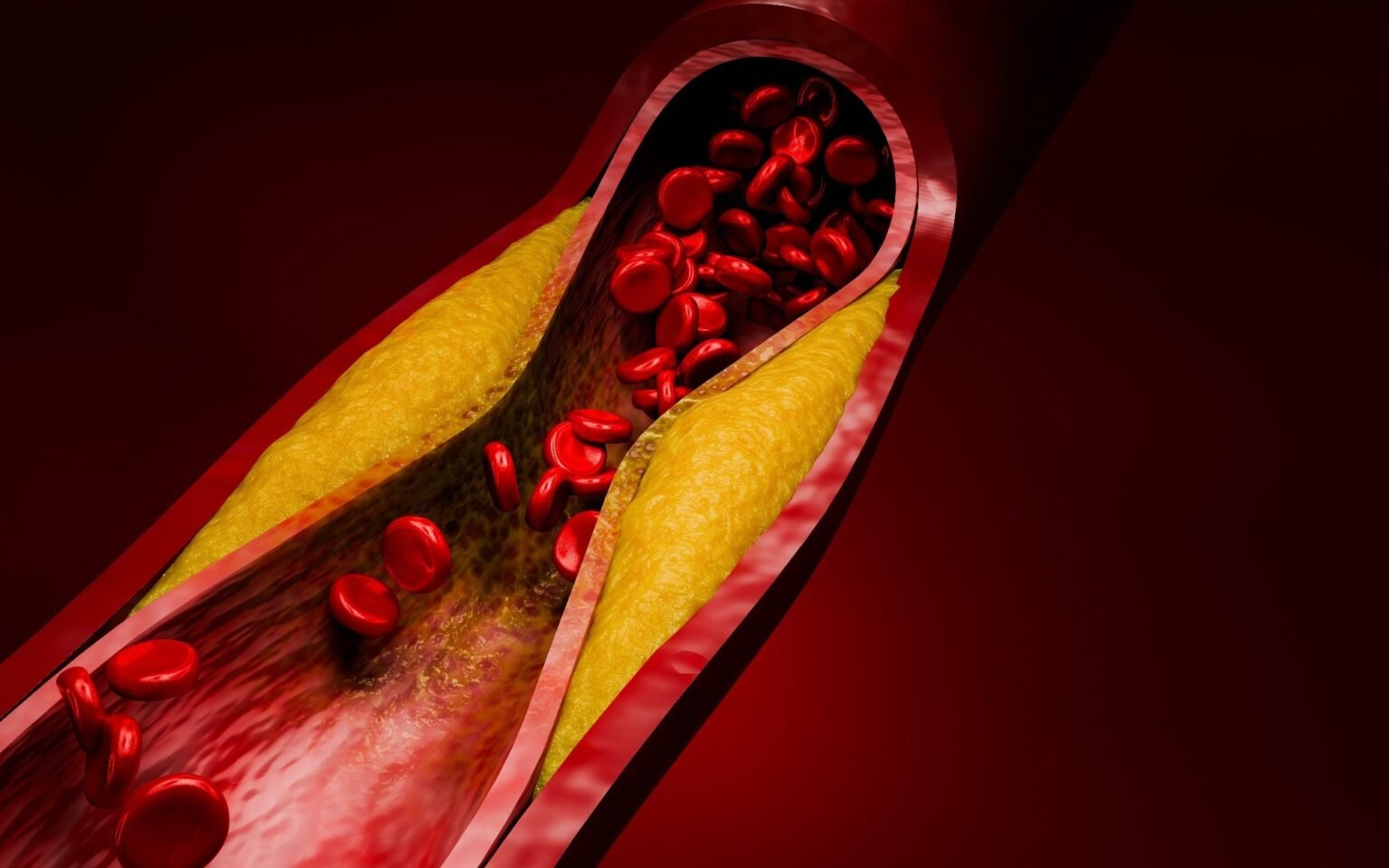
Key cholesterol guidelines were released just as pivotal new trial data was released, revealing that rapidly evolving evidence may soon change LDL goals and prevention strategies for high-risk patients.
Image credit: Ridersuperone / Shutterstock
recent guidelines and accompanying it editor A paper published in the Journal of the American College of Cardiology (JACC) highlighted that scientific discoveries can outpace the development of guidelines.
The American Heart Association (AHA) and American College of Cardiology (ACC) employ rigorous methodologies to develop clinical practice guidelines. They aim to produce the highest quality guidelines that are timely, clinically relevant, reliable, transparent, and accessible. Therefore, guideline development requires sufficient time for literature searches, expert consensus, development of recommendations, peer review, approval, and publication.
Therefore, it is not surprising that the pace of science sometimes exceeds the schedule for guideline development. This gap is exemplified by the publication of the Evolocumab Efficacy in Patients at High Cardiovascular Risk without History of Stroke or Myocardial Infarction (VESALIUS-CV) trial results compared to the 2026 ACC/AHA Guidelines for the Management of Dyslipidemia.
VESALIUS-CV study results in high-risk patients
VESALIUS-CV was a large, randomized, placebo-controlled trial of 12,257 patients at high cardiovascular risk but without a history of stroke or myocardial infarction (MI). Patients with coronary artery disease, peripheral artery disease, cerebrovascular disease, or at least moderate atherosclerosis according to coronary artery calcium (CAC) scores, and high-risk diabetic patients without a history of stroke or myocardial infarction on statin therapy, were randomly assigned to receive evolocumab or a placebo for more potent low-density lipoprotein cholesterol (LDL-C) lowering.
The trial had two primary endpoints: 1) a composite of coronary heart disease (CHD) death, ischemic stroke, or MI (3-point major adverse cardiovascular event, MACE), and 2) a composite of ischemia-induced arterial revascularization, CHD death, stroke, or MI (4-point MACE). In total, 67% of the population had no history of stroke or myocardial infarction and had qualifying atherosclerosis.
Of the two-thirds of the eligible population with atherosclerosis, 1,000 participants had a CAC score of 100 Agatston units (AU) or higher. Approximately 49% of the population had high-risk diabetes, of which 33% had high-risk diabetes without atherosclerosis. Evolocumab significantly reduced both endpoints, reducing LDL-C levels by an average of 55% over a median follow-up of 4.6 years.
The evolocumab group achieved a median LDL-C level of 45 mg/dL, while the placebo group achieved a median LDL-C level of 109 mg/dL. Absolute risk reductions of 1.8% and 2.8% were observed during follow-up for 3-point and 4-point MACE, respectively, with no difference in safety events between groups. The trial found no differences in outcomes between groups based on baseline LDL-C, disease of interest, or baseline lipid-lowering treatment.
2026 ACC/AHA Dyslipidemia Guidelines Recommendations
The 2026 guidelines replace the older ACC/AHA guidelines for blood cholesterol management and serve as a one-stop point for managing patients with dyslipidemia, including hypertriglyceridemia, high blood cholesterol, and elevated lipoproteins(a). The guidelines state that CAC testing with noncontrast cardiac CT may be considered for men 40 years and older and women 45 years and older when treatment decisions are uncertain in selected borderline or intermediate-risk adults. It also includes individualized CAC-based management recommendations for adults with asymptomatic coronary atherosclerosis.
Screening for dyslipidemia is recommended at age 2 years and older if there is a family history of juvenile atherosclerotic cardiovascular disease (ASCVD), familial hypercholesterolemia (FH), or severe hypercholesterolemia. Otherwise, it is recommended to repeat at age 9 to 11 years and again at age 19 years to identify FH and other lipid disorders.
Guidelines recommend estimating lipid levels 4 to 12 weeks after starting lipid-lowering treatment. An LDL-C goal <100 mg/dL is recommended for patients at borderline or intermediate risk initiating statin therapy. Depending on the specific clinical setting, CAC burden, and whether the patient has established ASCVD, goals of <70 mg/dL and <55 mg/dL are recommended for high-risk and very high-risk patients, respectively.
The guidelines state that LDL-C-lowering therapy can be considered as primary prevention of ASCVD for adults with an estimated 10-year predicted risk of cardiovascular disease events (PREVENT-ASCVD) of 3% to less than 5%. LDL-C-lowering therapy is also recommended for patients with PREVENT-ASCVD estimates of less than 5% to 10%, and at least moderate-intensity statin therapy is recommended for this intermediate-risk group.
Implications for future dyslipidemia guideline updates
The results of the VESALIUS-CV study have significant implications for the 2026 ACC/AHA guidelines, as they had not yet been discovered at the time of final review and approval of the new guidelines. Current guidelines distinguish between ASCVD patients who are at very high risk and those who are not.
However, the authors of the 2026 ACC/AHA guidelines note that in clinical practice, most patients with ASCVD are at very high risk, and only a minority are not. In the VESALIUS-CV trial, the cardiovascular benefits of intensive LDL-C lowering in patients without a history of stroke or myocardial infarction may blur current ASCVD risk distinctions when defining LDL-C goals.
Therefore, future updates to the guidelines in 2026 should include a single treatment pathway for all ASCVD patients with the optimal goal of achieving LDL-C levels below 55 mg/dL. The VESALIUS-CV trial also redefined the benefits of intensive LDL-C-lowering treatment for individuals with high-risk diabetes and at least one high-risk characteristic. The editorial also notes that this study strengthens support for recommendations to address moderate subclinical atherosclerosis, including an LDL-C goal of <70 mg/dL for CAC scores of 100 AU or higher and an optional target of <55 mg/dL for CAC scores of 300 AU or higher. Therefore, future guideline updates should also expand recommendations for this high-risk population.