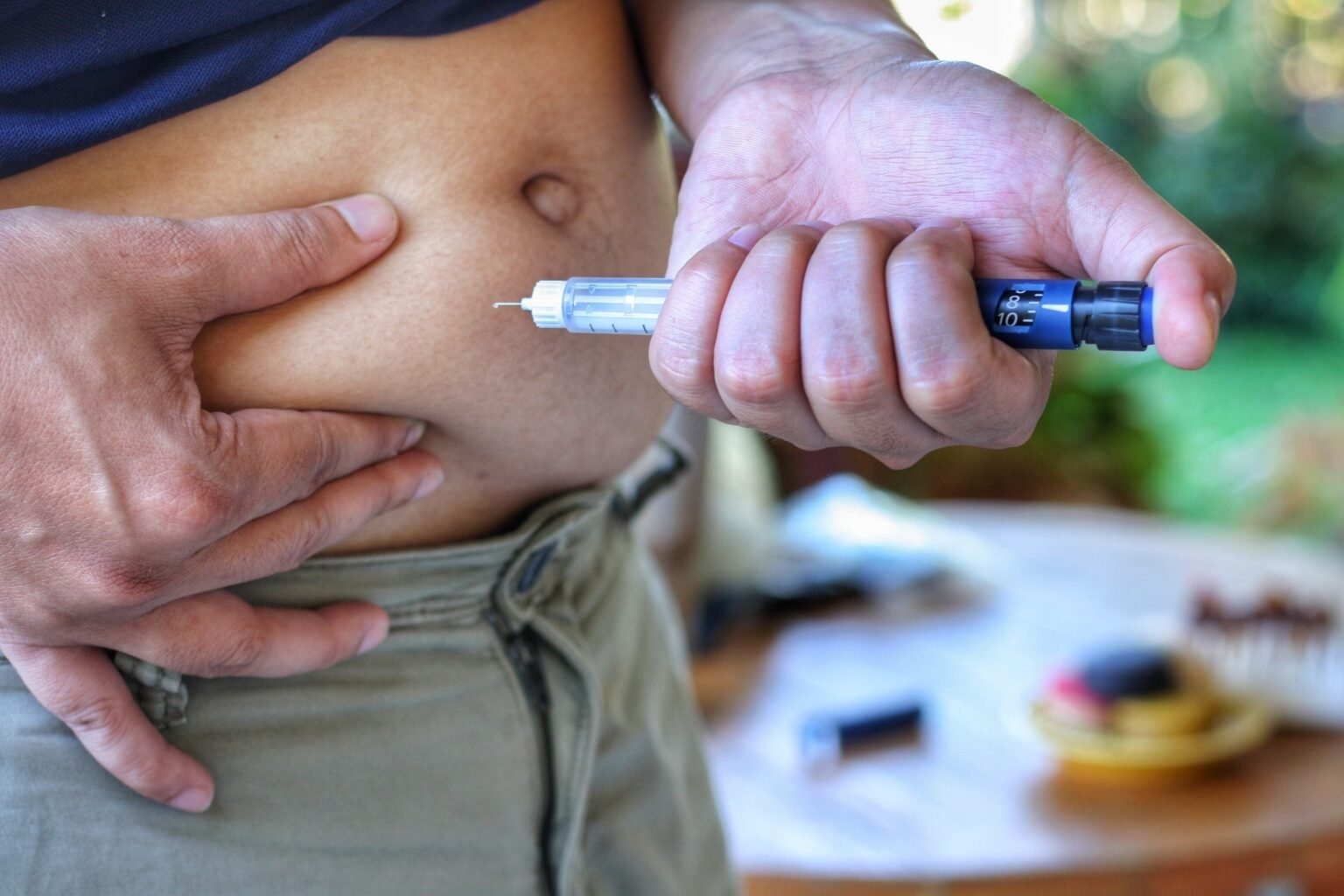
A large study of U.S. military veterans suggests that GLP-1 diabetes drugs may impact addiction-related outcomes and reveals a surprising association between metabolic treatment and substance use risk.
Study: Glucagon-like peptide 1 receptor agonists and risk of substance use disorder in U.S. veterans with type 2 diabetes: A cohort study. Image credit: Kotcha K / Shutterstock
In recent research, british medical journal Evidence suggests that commonly prescribed medications for type 2 diabetes (T2D) may be associated with a reduced risk of substance use disorders (SUD). These findings demonstrate an unexpected association between diabetes treatment and addiction risk.
Researchers investigated the effects of starting glucagon-like peptide-1 (GLP-1) receptor agonist (RA) therapy in U.S. veterans with T2D. They found that people who started taking these drugs had a lower risk of developing an SUD. Among people already living with such conditions, the drug was also associated with fewer adverse outcomes such as SUD-related hospitalizations, overdoses, and suicidal thoughts and attempts.
The results of this study highlight a potential new role for these diabetes treatments. However, further research is needed to confirm the broader clinical impact. SUDs remain a major health challenge among veterans.
Background: GLP-1 receptor agonists and brain reward pathways
GLP-1 RA drugs are widely prescribed for the treatment of T2D. Growing evidence suggests that these drugs may also affect brain pathways associated with addiction. Preclinical studies suggest that these drugs may cross the blood-brain barrier (BBB) and act on areas involved in reward, motivation, and impulse control. These behaviors can affect dopamine signaling in the brain’s reward circuits.
Preclinical studies have shown that GLP-1 RAs may reduce the reinforcing effects of substances such as nicotine, alcohol, opioids, and cocaine. Observational studies in humans have also reported a reduction in the risk of certain SUDs after starting treatment. However, evidence of broader benefits remains limited. Few large-scale studies have evaluated the potential role of the GLP-1 receptor agonist drug class in preventing or improving SUD outcomes.
Study design and veteran cohort
In this cohort study, researchers examined the association between GLP-1 RA and SUD in patients with T2D treated through the U.S. Department of Veterans Affairs (VA) health care system, which includes more than 1,000 outpatient clinics and 170 medical centers.
The study population included veterans with and without a history of SUD. All participants were active users of VA health care services, defined as having at least two clinical encounters and one pharmacy record in the year prior to enrollment. Researchers excluded individuals who had previously used GLP-1 RAs and those with drug contraindications such as gastroparesis, diabetic ketoacidosis, thyroid cancer, pancreatitis, severe hypoglycemia, or severe renal impairment.
Trial emulation of data sources and targets
The researchers emulated eight parallel targeted clinical trials within the framework of an active comparator. Seven of these analyzes assessed incident SUD development in 524,817 participants. One analysis focused on outcomes for 81,617 people with a history of SUD. In total, the team analyzed electronic medical record data from 606,434 participants.
The dataset included information on outpatient visits, hospitalizations, pharmacy records, vital signs, laboratory results, and Medicare data. The researchers also estimated the Area Deprivation Index (ADI), derived from participants’ residential address, to assess socio-economic status.
Research results and statistical analysis
Key study outcomes included the development of alcohol, cocaine, cannabis, opioid, and nicotine use disorders. Researchers assessed adverse outcomes among participants living with SUDs, including SUD-related hospitalizations, emergency department (ED) visits, overdoses, suicidal ideation, and SUD-related deaths. They compared these results to those observed after initiation of sodium-glucose cotransporter 2 (SGLT-2) inhibitors.
The research team followed the participants for up to three years. They used an inverse probability-weighted Cox survival model to estimate the hazard ratio (HR) and 3-year net risk difference (NRD) per 1,000 people for statistical analysis.
Results: Reduced risk of substance use disorder
Compared to the use of SGLT-2 inhibitors, initiation of a GLP-1 RA was associated with a reduced risk of alcohol use disorder (HR, 0.82; NRD, -5.57). GLP-1 RA initiation was also associated with reduced risk of cannabis use disorder (0.86; -2.25), cocaine use disorder (0.80; -0.97), nicotine use disorder (0.80; -1.64), opioid use disorder (0.75; -0.86), and other substance use disorders (0.87; -1.12). Combined study results including all new-onset SUDs showed similar results (0.86; -6.61).
Outcomes for individuals with pre-existing SUD
In individuals living with a SUD, the development of GLP-1 RA was associated with decreased SUD-related emergency department visits (0.69; -8.92), hospitalizations (0.74; -6.23), overdose events (0.61; -1.49), suicidal ideation (0.75; -9.95), and SUD-related mortality (0.50; -9.95). −1.52). Findings regarding treatment adherence were consistent with those observed for treatment initiation of new-onset SUD and associated adverse events in SUD patients.
Sensitivity analyzes using sulfonylurea initiators as controls, multiple lookback periods, overlapping weighting, mean treatment effects relative to controls, truncated cutoffs, and trimmed propensity score thresholds yielded similar results, supporting the robustness of the results.
Conclusion: Potential role of GLP-1 drugs in addiction prevention
The results of this study suggest that initiation of GLP-1 RA may provide benefits beyond glycemic control for T2D patients. These drugs were associated with a lower risk of new-onset SUD and associated adverse outcomes such as overdose, hospitalization, and suicidal ideation in people living with SUD. This result highlights the potential role of GLP-1 RA in the prevention and management of SUD.
Clinically, this finding may inform therapeutic considerations, especially for diabetic patients at risk for or experiencing SUD. However, clinicians must weigh the potential benefits against known side effects, highlighting the need for further research and individualized clinical decision-making. Because this is an observational study conducted in a primarily older male veteran population, the results cannot establish causality, may not be fully generalizable beyond the VA health care system, and residual confounding cannot be excluded despite statistical adjustments.
Reference magazines:
- Miao Kai, Taeyeon Choi, Yang Shi, and Ziyad Al-Aly. (2026). Glucagon-like peptide-1 receptor agonists and the risk of substance use disorder in US veterans with type 2 diabetes, a cohort study. British Medical Journal, 392. DOI: 10.1136/bmj-2025-086886, https://www.bmj.com/content/392/bmj-2025-086886